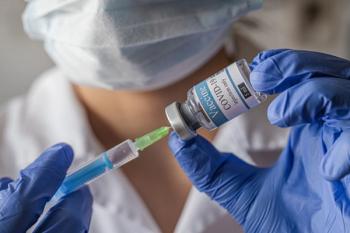
The Importance of COVID-19 Booster Shots
A panel of experts gives an overview on the purpose of COVID-19 booster shots and their critical importance to population health.
Episodes in this series

Peter Salgo, MD: Hello everyone and welcome to this Peer Exchange titled, “COVID-19: Expectations on the Rollout of Booster Shots.” I am Dr Peter Salgo; I’m a professor of medicine and anesthesiology at Columbia University Vagelos College of Physicians and Surgeons here in New York City. I am pleased to tell you that joining me today are some of my colleagues: Dr Donald Alcendor, associate professor of microbiology and immunology at Meharry Medical College, adjunct associate professor of pathology, microbiology, and immunology at Vanderbilt University School of Medicine in Nashville; Dr Jeff Goad, associate dean of academic affairs, professor and chair of the Department of Pharmacy Practice at Chapman University School of Pharmacy, in Irvine, California; Dr Jason Gallagher, clinical professor, clinical specialist, infectious diseases, and director of the PGY2 Residency in Infectious Diseases Pharmacy at the Temple University School of Pharmacy, in Philadelphia; and Dr Angela Rasmussen, research scientist III at the Vaccine and Infectious Disease Organization in Saskatchewan, Canada. Thank you all for joining us, it’s terrific to have you here today. Why don’t we start with the basics; we’re dealing with COVID-19. It seems that at some point or another everybody is in information and volume overload. The population has been hearing about COVID-19 for 2 years. Why don’t we cut to the chase and try to get down to some very bare-bones facts. What is the purpose of a COVID-19 booster, and why is the booster itself important? Who wants to start us off, Donald?
Donald Alcendor, PhD: The purpose of the COVID-19 booster is to give people an added level of protection from COVID-19 if their existing protection has waned over time. The booster would potentiate their immune system to bring them back up to a level of protection that would protect them from infection, hospitalizations, and death, which the vaccine is designed to do.
Peter Salgo, MD: You know what people are saying though, right? “I’ve got 2 shots; now you’re telling me I’m going to have a third. When are you going to drop the other shoe, or the fourth shoe, and tell me I need a fourth, fifth, or a sixth booster?” Anybody can answer this: is there an end to this cycle in sight?
Angela Rasmussen, PhD: I think there is. We have many vaccines that are multiple shot regimens that require multiple boosts. A lot of people want to talk about influenza vaccines, but influenza is really a very different virus. There are multiple strains and subtypes circulating, so you need to be boosted but also vaccinated for some of these other strains. With SARS-CoV-2, as with many other viruses, including the measles virus and the inactivated polio vaccine, many vaccines are multiple shot regimens; hepatitis B vaccine is another example of that. It’s probably correct that we will get to a point where you’ve been sufficiently boosted, that you have very responsive protective long-term memory immunity to this virus. Because these vaccines were expedited to the clinic, we don’t really know what the optimal dosing regimen is, but I think it’s very unlikely that we’re going to be needing COVID-19 boosters every 6 months for the rest of our lives.
Peter Salgo, MD: Do you think it is a factor of the unique nature of these vaccines, the mRNA vaccines versus other biologics that work differently?
Angela Rasmussen, PhD: It could be. The mRNA vaccines are a different technology platform, same with the adenovirus-vectored vaccines; they don’t fundamentally work any differently as far as your immune system is concerned though. They just expose your immune system to the antigen, in this case the spike protein from SARS-CoV-2 the same way that a protein subunit vaccine would, and the same way that an inactivated virus would. I don’t that there’s anything fundamentally different to this technology that would necessitate constant boosters. Certainly the data that we do have suggest that there are immune responses to these vaccines, both the mRNA and the adenovirus-vectored vaccines, that are compatible with long-term memory immunity. Therefore, I wouldn’t anticipate that that’s going to be a feature of this particular technology platform.
Peter Salgo, MD: To all of you then, let’s talk about the role that the booster shots are playing in strengthening the immune response. Is it just that they’re kick-starting it once again, or is there something uniquely different in the third shot compared to the first 2? Does anybody have a view on that?
Jeff Goad, PharmD, MPH: One thing to add on to what Angie was saying too is if you look at the natural disease, we don’t see lifelong immunity from natural disease either. I think what we’re seeing is that the human is just not able to develop a long-lasting response, whether we’re using vaccine or natural disease. When you start talking about the role of the booster and how many we may need going forward, I think a lot of it has to do with how well we do with getting the primary series in, and at least now getting the booster in 6 months later, because vaccination to herd immunity is going to be critical moving forward.
Peter Salgo, MD: I want to thank you at home for watching this Peer Exchange discussion. If you enjoyed the content, subscribe to our e-newsletters to receive upcoming Peer Exchanges and other great content right in your inbox.
Transcript edited for clarity.