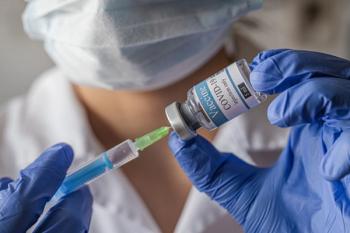
Safety and Efficacy of COVID-19 Booster Shots
Dr Peter Salgo leads a discussion on the safety and efficacy of COVID-19 booster shots with a comparison to historical vaccine rollouts.
Episodes in this series

Peter Salgo, MD: Let’s keep discussing safety. What does the evidence suggest about the safety and efficacy of the booster shots across the various manufacturers? Donald, is there any difference?
Donald Alcendor, PhD: When you look at the second shot or the first shot of the Johnson & Johnson, side effects that might occur are side effects that are very similar to the initial doses. They don’t see anything that’s dramatically added in terms of side effects. However, this is from person to person and can change from one individual to another. Again, a person could experience a severe adverse event with any of these vaccines.
Peter Salgo, MD:One of the things that was clear to me is that when there wasn’t a lot of media attention on any vaccination program, the number of people who had severe side effects was calculated, documented, and we went forward. If it was more than what we thought was reasonable, things changed. Here, the instant there’s an adverse reaction anywhere, it is front-page news. People don’t have the experience of seeing vaccine rollouts before. Whether it’s clots, neurologic complications, myocarditis, they don’t necessarily have the statistical background to evaluate this is 1 in a 1,000,000, 1 in 10,000,000, 1 in a 100,000. What does this really mean? What are my chances? How do you combat that? How do you deal with that?
Donald Alcendor, PhD: You want to try to explain to them that we have been taking vaccines for decades. I talk to parents all the time. I explain to parents about their experience with vaccines, and they have quite a bit. I ask them, “Do you have a child that goes to public school?” They tell me yes. I say, “To go to public school there’s state mandated vaccinations that they have to have, and they have to be updated every year.” I ask them, “How many of your children come back after receiving a vaccine and complain of an adverse event?” I don't hear anything. The reason being is that vaccines have been safe and effective for decades. Vaccines have allowed us to live they say 30 years longer in part to vaccines than we did 100 years ago. Vaccines are the most highly scrutinized public health interventions we know. When you think about vaccines and what they go through, you’re talking about 3 phase clinical trials, a data safety monitoring board, the FDA [Food and Drug Administration] advisory committee, the FDA, then the CDC [Centers for Disease Control and Prevention] specific advisory committee, and then at a P4 level of pharmacovigilance that follows people that get vaccines for years after.
Jeff Goad, PharmD, MPH:Currently too, to follow up what you’re saying, is that when you talk about statistics people’s eyes glaze over. Where are they really getting their information? Facebook? Instagram? I think one of the things we must do is when you have your patients who took their 5-year-old, 6-year-old, they didn’t say anything. Their arm didn’t even hurt. That needs to go on social media. Because guess what’s showing up there? “My arm hurt. I got some weird reaction that people associate with vaccine.” That’s all they’re seeing. Therefore, we must encourage our patients post this stuff on social media: “My kid got vaccinated, it was fine.”
Peter Salgo, MD:Let me give you a personal story, it also discloses a bit of how old I am. Back in the 1950s, I remember my parents saying you can’t go to a public swimming pool in the summer. You can’t do it. Polio, the scourge of this country, is everywhere. Then along came Jonas Salk. People brought their kids in. I got one of the first waves of polio vaccine. I got jabbed in the arm in the gym in my public school. My parents praised the name of Jonas Salk, and he was a secular god in this country. There were side effects of the polio vaccine, and there were side effects to the Sabin vaccine. Today is different. What’s so different now? Why aren’t people saying, “God bless this vaccine?” What has changed?
Angela Rasmussen, PhD:I think if you want to compare it to the polio vaccine, and I talked to my mom about her experience because I think she may be around your age, Peter.
Peter Salgo, MD:Thanks a lot, Angie. Let’s just let one go.
Angela Rasmussen, PhD:I took my polio vaccine for granted. I’m old enough that I did get an oral polio vaccine when it was still used in the U.S. I actually remember it even though I was only 2 because I just remember getting a ton of shots and then I got a sugar cube. I asked my mom, “Did you get a shot or a sugar cube?” and she said, “Yes. I got a sugar cube.” My parents couldn’t wait to get me in there. But if you go back even further, my mom told me something else: she said it was way better than the smallpox vaccine, and talk about a vaccine with a bad profile in terms of adverse events. At the same time, nobody talks about the smallpox vaccine as if it were unnecessary. In fact, thanks to that vaccine, we don’t have to get smallpox which has a mortality rate of upwards of 30%.
Peter Salgo, MD:It’s very brutal.
Angela Rasmussen, PhD:It’s terrible. We had smallpox come back for some reason; it was a lab leak. I would not hesitate to get a vaccine myself. I think that it’s all relative. When you don’t grow up seeing your friends paralyzed, seeing your friends in an iron lung; when you don’t grow up seeing children all over the place getting sick and sometimes dying from a preventable illness, then I think you do start to get a little complacent. I think as a society we have gotten complacent about some of these viruses. We hear this in anti-vaccine propaganda all the time. Measles; it’s a childhood disease. It’s natural. It’s not a problem. It doesn’t kill that many kids. But back in that day when measles was rampant, people did not think twice about a vaccine that would prevent it.
Peter Salgo, MD:I want to put a cap on this, which is you say that we’re not seeing people get sick from measles or mumps or smallpox. However, this pandemic is killing hundreds of thousands in the U.S., and across the globe millions of people. The message, the takeaway, is different here than it was with polio. Why?
Donald Alcendor, PhD: I think we must go back and just understand the extent of coronaviruses as we know it. That is there are 7 different coronaviruses that infect humans. Many of them are nonpathogenic. The last 3 are very important because they can produce a mortality rate for SARS COVID-1 10%, COVID-2 about 3%-5% percent. However, the MERS [Middle East respiratory syndrome] virus, which is a very dangerous coronavirus, has a fatality rate of 35%. When we think about it, we have never seen any variants that have developed from the common circulating coronaviruses in children. We were simply surprised by this. Our bodies have never seen this virus. Remember, this is a zone not a transmission. The idea is a zoonotic virus, and again its primary host more than likely is the bat. The secondary intermediate zoological host is currently unknown to this day; we just haven’t seen this. The way we can track this in the same way in history, is we look at the Spanish flu where young people had not seen that virus and had a tremendous amount of mortality in younger folks and not in younger folks that had seen that virus prior. It has to do with your immune recognition of something. If your immune symptom has something to go on, then it’s going to be better equipped to fight it. We had nothing to go on with this the SARS coronavirus.
Peter Salgo, MD: I want to thank you at home for watching this Peer Exchange discussion. If you enjoyed the content, subscribe to our e-newsletters to receive upcoming Peer Exchanges and other great content right in your inbox.
Transcript edited for clarity.
Newsletter
Stay informed on drug updates, treatment guidelines, and pharmacy practice trends—subscribe to Pharmacy Times for weekly clinical insights.