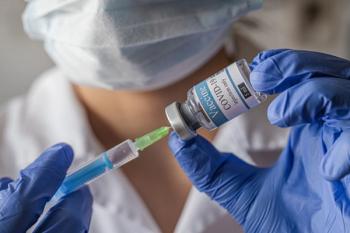
How COVID-19 Booster Shots Affect Herd Immunity
Dr Jason Gallagher explains how COVID-19 booster shots affect herd immunity in the United States.
Episodes in this series

Peter Salgo, MD: All right, let’s ask some basic questions. First, can we just have a vote? Is the booster necessary to maintain immunity, or will we settle out without it at some immune level that is satisfactory? Who wants this one, Jason maybe?
Jason Gallagher, PharmD, FCCP, FIDP, FIDSA, BCPS: That’s not exactly a layup, Peter.
Peter Salgo, MD: That’s why I gave it to you; you’re good, come on.
Jason Gallagher, PharmD, FCCP, FIDP, FIDSA, BCPS: I look at vaccines on 2 different levels: what’s best for the public health and what’s best for the individual. I think from an individual standpoint, there’s no doubt that a booster is beneficial. From a public health standpoint, if we have infinite numbers of supply of vaccine that we can give to anybody, then yes, the optimal way to do it is to vaccinate and boost the entire plant. If I could shift where 1 particular dose goes, I’d be shifting it to a country or a person who hasn’t received their first vaccines yet. I want to go back a little to what Angie and Jeff have already introduced here; I think one of the things that is unique about this isn’t the platforms themselves, and the immune system doesn’t see it any differently. It’s deploying it in the middle of an active pandemic. We’re trying to shift the end point as we’re going and change the trajectory of the pandemic. When was the last time we’ve done that actively with vaccines? Truthfully, we are learning as we go.
Peter Salgo, MD: What is the primary goal of the vaccine? You alluded to this, and I want to parse that out before we move on. Is the primary goal of this vaccine to protect the individual? Or is the primary goal of this vaccine to protect society, to get a certain amount of immunity as a baseline until the entire virus is tamped down?
Donald Alcendor, PhD: The primary goal of this vaccine is protection from severe disease, hospitalizations, and death. When you think about those primary goals, this vaccine as we look at it, that came from the initial sequence of the spike glycoprotein, it has done that with the current viruses of concern. That is, it has done it with the Alpha, Beta, Delta variants; we don’t know if it’s going to do it with Omicron as well. Being able to protect from severe disease, hospitalizations, and death, if any vaccine can do that, it’s a good vaccine. This vaccine has yet to let us down in that regard.
Peter Salgo, MD: We’ve got both an altruistic aspect of getting vaccinated, which is helping to protect the entire population, and a very selfish benefit, which is it’s going to protect you from severe disease and potential death. If that’s what we’re looking at, what is the outlook then for achieving herd immunity with vaccination alone in the United States?
Donald Alcendor, PhD: I think what we’d have to look at is where we are right now. We’re looking at more than 40 million people who are eligible to get a vaccine who are unvaccinated as we see now. I live in Tennessee; Tennessee has 95 counties, 70 of those are rural counties. There’s a tremendous amount of vaccine hesitancy and vaccine resistance in those counties; I don’t see that going away. We are also dealing with anti-vaxxers who are putting out misinformation and helping support conspiracy theories around ill-found ideas about vaccine efficacy and safety. If we look at where we are, we have to say that herd immunity might have to be taken off the table at this point. The reason being is that we are getting breakthrough infections, and we are getting the evolution of variants that we don’t know if we can control with existing immunity. So we are in a holding place when it comes to herd immunity. When you think of herd immunity, for COVID-19 we’re talking about 75% to 85% of people in the United States being vaccinated. Now, if you think you can achieve that, then ask yourself this, what about the developing world? We are a global community and not just a United States community. We are not safe until all of us are vaccinated, that is, the global community vaccinated.
Peter Salgo, MD: There is the Omicron variant coming out of Africa. One of the things that is transparent to me is that Africa is undervaccinated, and they haven’t had the access to the vaccine that the first world has had. Doesn’t that make your point? If we could vaccinate everybody, we’d all be safer?
Donald Alcendor, PhD: Those countries cannot afford vaccine contracts. Vaccine contracts are paid for before the vaccine is even made. You’re looking at rich countries having more than 60% of the vaccine supply. What you need to do is this: you need to bring vaccine manufacturing and distribution local to those communities, and that must be done through public-private partnership with vaccine companies and the governments. The World Health Organization must be involved.
Peter Salgo, MD: I want to thank you at home for watching this Peer Exchange discussion. If you enjoyed the content, subscribe to our e-newsletters to receive upcoming Peer Exchanges and other great content right in your inbox.
Transcript edited for clarity.