Commentary
Article
Time to Address the Management of Antiphospholipid Syndrome
Author(s):
It is vital for health care teams to recognize the signs and symptoms of antiphospholipid syndrome and to identify the severity of a patient’s diagnosis based on their aPL profile.
Background: Epidemiology and Etiology
Antiphospholipid syndrome (APS) is an autoimmune disorder characterized by thrombotic or obstetrical complications due to the presence of antiphospholipid antibodies.1 These antibodies target a specific plasma protein in the body called B2-glycoprotein I that binds to phospholipid surfaces.
Image credit: shidlovski | stock.adobe.com

Once the antibodies bind to the B2-glycoprotein, it results in an up-regulation of prothrombotic adhesion molecules—E-selectin and tissue factor. The prevalence of antiphospholipid antibodies is not well established in the general population.
However, a 2019 population-based study that looked at 33 cases of APS from 2000 to 2015 demonstrated APS occurring in 2 persons per 1,000,000 per year, with an estimated prevalence of 50 per 1,000,000 per year.2
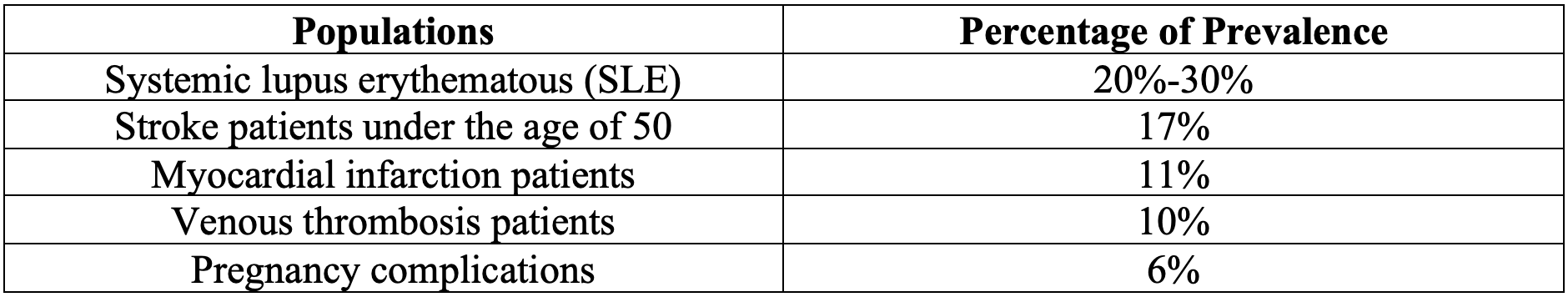
The following table depicts the percentage of prevalence for certain populations of people with antiphospholipid antibody profiles:3,4
Table. Prevalence for certain populations of people with antiphospholipid antibody profiles.

Clinical Presentation
The following table demonstrates common clinical signs of APS:1,5
Table. Common clinical signs of APS
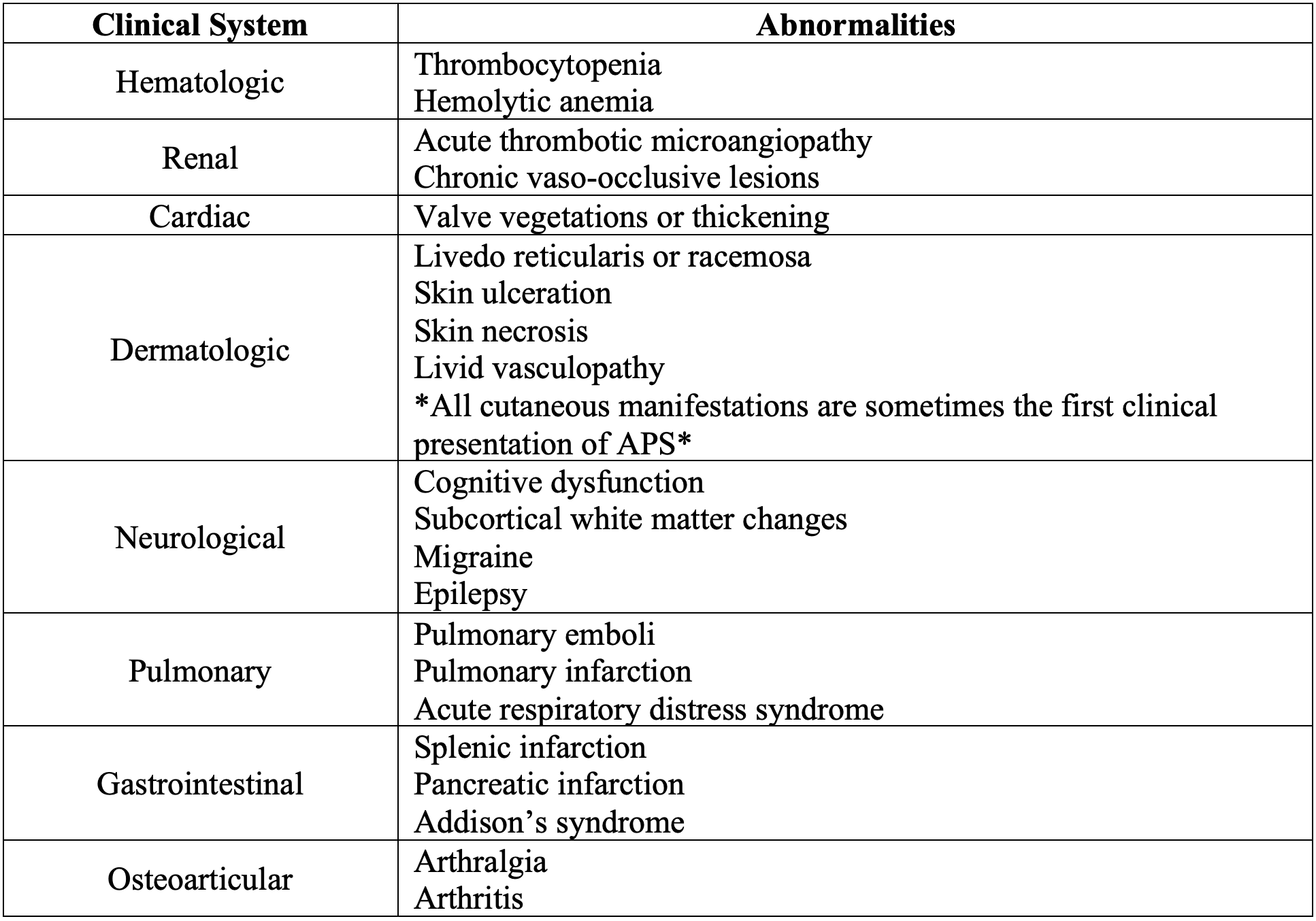
Diagnosis and Risk Stratification
Diagnosis is done based on the revised Sapporo Classification criteria for APS.6 In diagnosing patients, they can be stratified into different categories for the development of thrombotic events, including high-, moderate-, and low-risk:
Table. Diagnosing APS

Management of APS
The following table demonstrates management strategies from select guidelines:7
Table. Management strategies for APS.
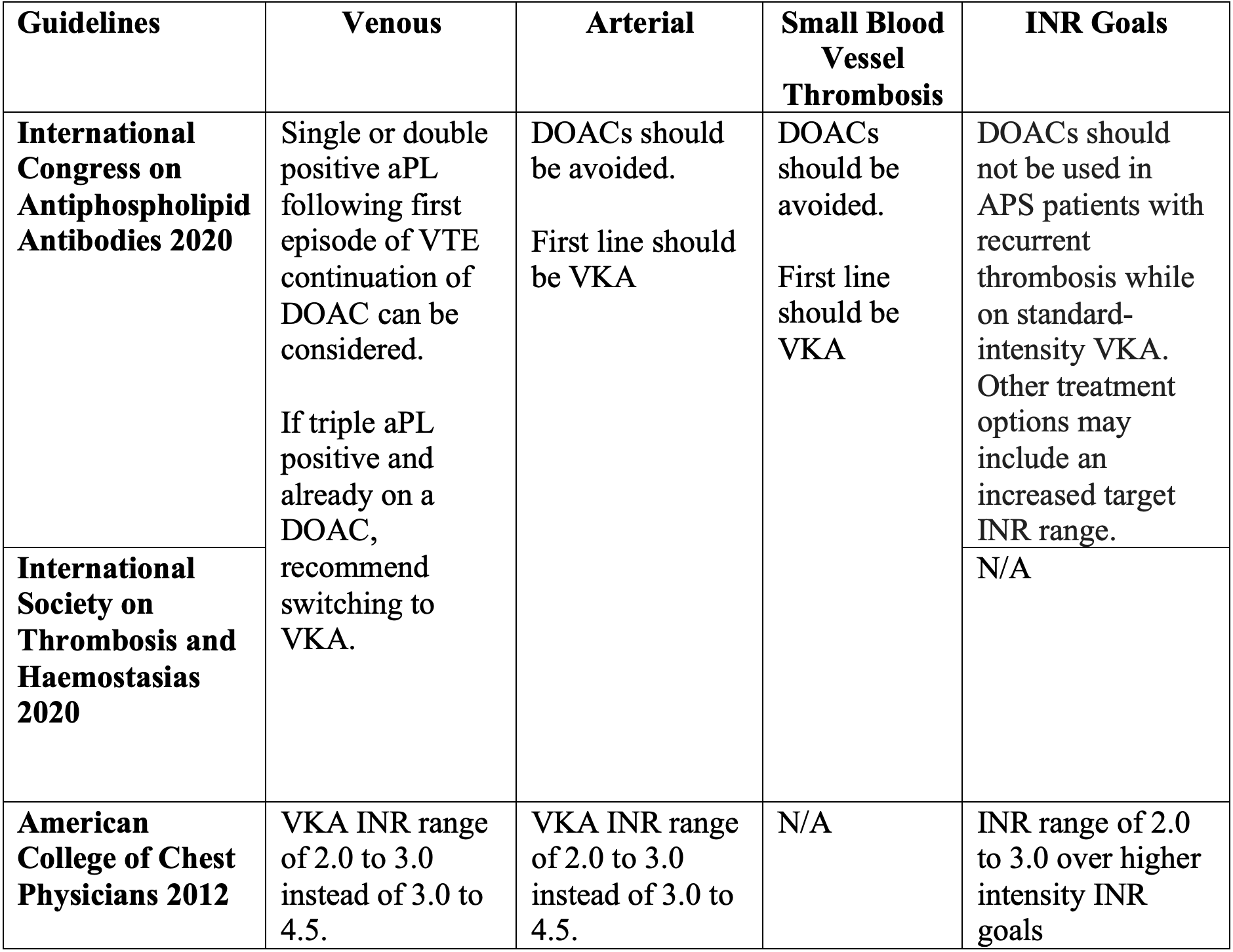
A 2023 meta-analysis by Khairani and et al was conducted to examine the safety and efficacy of direct oral anticoagulants vs warfarin in patients with APS. The meta-analysis included 4 open randomized control trials of 472 patients.8
Overall, the odds of subsequent VTE, and major bleeding was not significantly different between the 2 treatment groups, yet patients with APS randomized to DOACs compared to VKAs had an increased odd of subsequent arterial thrombotic events, particularly stroke.
Conclusion
APS is a rare autoimmune disorder that requires proper medical management. With a morality rate that is 50%-80% higher than the general population, it is vital for health care teams to recognize the signs and symptoms of APS and to identify the severity of a patient’s diagnosis based on their aPL profile.9
In looking at the literature that we have in treating APS, there is a moderate consensus that vitamin K antagonist should be the first-line agents used in patients with thrombosis of the venous, arterial and small blood vessels, yet DOACS can be considered as an option in patients with single or double positive aPL profile with their first episode of VTE. The evaluation of efficacy with anticoagulation treatment is variable, for there is conflicting literature on the INR goals for patients with APS: 2.0–3.0 vs 3.0–4.0.
Clinical judgement is needed in determining the INR goal with certain factors guiding clinical decisions, including number of recurrent thrombosis and aPL profiles.
About the Author
Author: Jamie Rusan, PharmD Candidate, Drake University Class of 2023
Preceptor: Lauren Stonerock, PharmD
References
1. Garcia, D., & Erkan, D. (2018). Diagnosis and Management of the Antiphospholipid Syndrome. The New England journal of medicine, 378(21), 2010–2021. https://doi.org/10.1056/NEJMra1705454
2. Duarte-Garcia A, Pham M, Crowson C, et al. 189 Epidemiology of antiphospholipid syndrome: a population-based study
Lupus Science & Medicine 2019;6:doi: 10.1136/lupus-2019-lsm.189
3. Ünlü O, Zuily S, Erkan D. The clinical significance of antiphospholipid antibodies in systemic lupus erythematosus. Eur J Rheumatol. 2016 Jun;3(2):75-84. doi: 10.5152/eurjrheum.2015.0085. Epub 2015 Dec 29. PMID: 27708976; PMCID: PMC5042235.
4. Andreoli, L., Chighizola, C. B., Banzato, A., Pons-Estel, G. J., Ramire de Jesus, G., & Erkan, D. (2013). Estimated frequency of antiphospholipid antibodies in patients with pregnancy morbidity, stroke, myocardial infarction, and deep vein thrombosis: a critical review of the literature. Arthritis care & research, 65(11), 1869–1873. https://doi.org/10.1002/acr.22066
5. Cervera, R., Piette, J. C., Font, J., Khamashta, M. A., Shoenfeld, Y., Camps, M. T., Jacobsen, S., Lakos, G., Tincani, A., Kontopoulou-Griva, I., Galeazzi, M., Meroni, P. L., Derksen, R. H., de Groot, P. G., Gromnica-Ihle, E., Baleva, M., Mosca, M., Bombardieri, S., Houssiau, F., Gris, J. C., … Euro-Phospholipid Project Group (2002). Antiphospholipid syndrome: clinical and immunologic manifestations and patterns of disease expression in a cohort of 1,000 patients. Arthritis and rheumatism, 46(4), 1019–1027. https://doi.org/10.1002/art.10187
6. Keeling, D., Mackie, I., Moore, G. W., Greer, I. A., Greaves, M., & British Committee for Standards in Haematology (2012). Guidelines on the investigation and management of antiphospholipid syndrome. British journal of haematology, 157(1), 47–58. https://doi.org/10.1111/j.1365-2141.2012.09037.x
7. Sayar, Z., Moll, R., Isenberg, D., & Cohen, H. (2021). Thrombotic antiphospholipid syndrome: A practical guide to diagnosis and management. Thrombosis research, 198, 213–221.
8. Khairani C, Bejjani A, Piazza G, et al. Direct Oral Anticoagulants vs Vitamin K Antagonists in Patients With Antiphospholipid Syndromes. J Am Coll Cardiol. 2023 Jan, 81 (1) 16–30. https://doi.org/10.1016/j.jacc.2022.10.008
9. Dabit, J.Y., Valenzuela-Almada, M.O., Vallejo-Ramos, S. et al. Epidemiology of Antiphospholipid Syndrome in the General Population. Curr Rheumatol Rep 23, 85 (2021). https://doi.org/10.1007/s11926-021-01038-2
Newsletter
Stay informed on drug updates, treatment guidelines, and pharmacy practice trends—subscribe to Pharmacy Times for weekly clinical insights.






