News
Article
Supplements
Impact of the Inflation Reduction Act on Vaccinations: What Pharmacists Need to Know
Author(s):
By educating their patients on the provisions of the Inflation Reduction Act, pharmacists can have an even greater impact by increasing vaccine uptake in historically underserved groups.
The Inflation Reduction Act (IRA)— signed into law by President Joseph R. Biden on August 16, 2022—is a landmark piece of legislation that aims to curb inflation by reducing the federal government’s budget deficit.1,2 Included in the bill are provisions that will take significant action on some of the most crucial challenges facing the American public: climate change and the rising costs of health care and prescription drugs.1 The IRA will address these concerns by lowering prescription drug prices, extending subsidies to help people pay for health insurance, and investing in domestic energy production while promoting clean energy.2 The long-awaited bill is financed largely by tax code reforms intended to raise the minimum tax on large corporations and improve taxpayer compliance by funding the IRS.1,3
Vitalii Vodolazskyi - stock.adobe.com

The bipartisan effort falls short of the goals of the Build Back Better (BBB) Act, which included more substantial changes to the tax code; the creation of a federal paid family and medical leave program; and measures to bring down the costs ofchildcare, housing, and home health care.4,5 The BBB Act was passed by the House of Representatives in November 2021, but it was stalled in the Senate due to lack of bipartisan support and some Democratic intraparty opposition.5 Although the BBB Act failed to pass both houses, many parts of its framework were successfully incorporated into the IRA, and it will have wide-ranging effects on the health care landscape starting as early as this year (2023).2,5
Health Care Provisions of the IRA
The IRA legislation carries forward the vaccine provisions from the BBB Act and delivers increased access and elimination of cost-sharing for vaccines to patients enrolled in Medicare Part D, Medicaid, and the Children’s Health Insurance Program (CHIP).2 These policy changes will enable more than 64 million seniors and people with disabilities to have coverage for adult vaccines without cost-sharing, finally achieving parity with nongrandfathered commercial, employer-sponsored, or health marketplace plans under the Affordable Care Act (ACA) (See Table).2,6-8
Image From the September 2023 Issue of Immunization Guide for Pharamcists
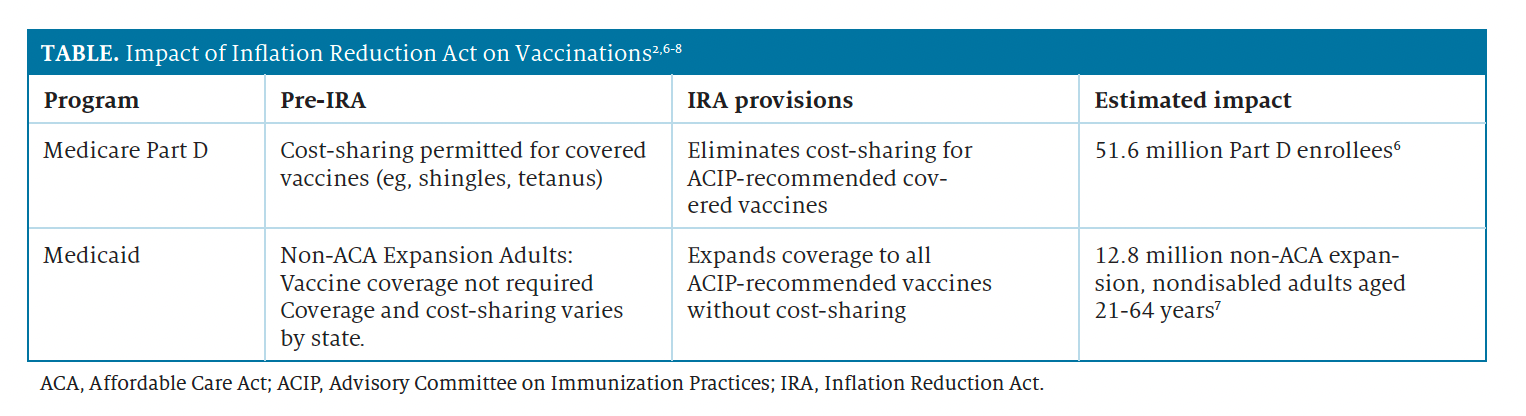
Under the IRA, effective as of January 2023, Medicare Part D plans may no longer impose cost-sharing for vaccines recommended by the Advisory Committee on Immunization Practices (ACIP).2 Part D plans may not apply a deductible, coinsurance, or any other cost-sharing requirement for these vaccines. ACIP-recommended vaccines covered under Medicare Part D include9:
- shingles;
- tetanus/diphtheria (Td);
- tetanus/diphtheria/pertussis (Tdap);
- hepatitis A; and
- hepatitis B.
Influenza, pneumococcal, COVID-19, and certain other vaccines were already covered without cost-sharing under Medicare Part B.9 Starting in October 2023, the IRA will address gaps in adult immunization coverage under Medicaid and CHIP.2,10 Medicaid enrollees include families under a certain income threshold, qualified pregnant women, and individuals receiving supplemental security income.11 Without a federal mandate, vaccine coverage is determined by individual states, and cost-sharing can vary greatly.12 The ACA and subsequent regulations have improved access by mandating vaccine coverage without cost-sharing for the Medicaid expansion population: nonelderly adults with an income up to 138% of the federal poverty level for states that have chosen to adopt the ACA Medicaid expansion.8 As of March 2023, 41 states, and the capital city of the District of Columbia, have expanded Medicaid.8 The IRA creates parity between Medicaid and Medicaid expansion programs by mandating coverage of ACIP-recommended vaccines, much like the existing coverage standards for the commercial insurance market. These new requirements will secure access to recommended vaccines for all Medicaid-enrolled adults and CHIP enrollees 19 years or older by requiring states to provide coverage without cost-sharing, thereby closing long-standing gaps in adult vaccine coverage in the United States.2
In addition to improving access to adult immunizations, the IRA will deliver lower prescription drug costs for people with Medicare, reduce drug spending by the federal government, and expand Americans’ eligibility and access to health insurance coverage.2 For the first time, starting in 2026, it will allow Medicare to negotiate with manufacturers for prescription drug prices by establishing a Drug Price Negotiation Program for certain single-source chemical drugs and biological products covered under Medicare Part B and Part D.2 The drugs selected for negotiation will have the highest total Medicare spending, and new medications will be selected for negotiations each year, starting with 10 drugs in 2026 and increasing to 20 drugs for 2029 and beyond.2 Effective January 2023, for certain medications covered under Part D, the IRA requires drug companies to pay annual rebates to Medicare if they increase the prices faster than the rate of inflation.2 Also effective January 2023, the IRA set a $35 cap on monthly Medicare enrollee cost-sharing for insulin.
Starting in 2025, the Part D benefit will be reconfigured to cap annual out-of-pocket spending to $2000, compared with current coverage, which has no limit on the total amount that beneficiaries pay out-of-pocket each year.2,13 For those who meet income eligibility criteria, the IRA extends premium subsidies for health plans sold on exchanges through 2025.2 Starting in 2024, the Act expands eligibility for the Part D Low-Income Subsidy Program. These key health care provisions of the IRA will have the potential to make a meaningful difference in the lives of millions of Americans, ensuring certain drugs and vaccines are more accessible, and therapies like insulin are more affordable.
Vaccine Provisions in the IRA: Patient Impact
Challenges to improving adult immunization rates and reducing vaccine-preventable diseases (VPDs) persist in the United States.14,15 Annual expenditures for the treatment of VPDs in adults are estimated at nearly $27 billion, with substantial downstream effects on health care utilization.14 Immunization as a public health initiative is one of the most cost-effective health care interventions, resulting in decreased incidence of VPDs and associated morbidity and mortality, shorter hospital stays, and reduced courses of treatment.14-16 Despite the abundance of evidence demonstrating the benefits of vaccination for VPDs, adult vaccination rates remain low for most routinely recommended vaccines, such as influenza and pneumococcal disease.17 Furthermore, the United States has failed to meet many of its Healthy People 2020 targets for vaccinating adults; vaccination rates will continue to be an objective for Healthy People 2030.18,19
Disparities in vaccination status among adults exist across race, ethnicity, and socioeconomic status; immunization rates for most vaccines are low among minority groups and people who are at lower income levels.20-22 For most vaccines, coverage remains higher among adults with private health insurance compared with groups who receive public health insurance.17 Affordability factors into vaccine nonadherence as well, with research demonstrating that reduced out-of-pocket costs improve vaccination rates.23
Provisions set forth in the IRA address coverage and cost-sharing obstacles to immunizations. In 2021, 3.4 million people received vaccines under Medicare Part D, with out-of-pocket costs totaling $234 million, or about $70 per enrollee.9,24 The most commonly administered Medicare Part D−covered vaccine is for the prevention of shingles; it accounted for 90% of all out-of-pocket Part D vaccine spending in 2021. In addition to being the most utilized, it is the most expensive, with some seniors paying almost $200 per immunization (2-dose series).9 Under the IRA, Medicare Part D enrollees will pay $0 out-of-pocket for these vaccines, which should make them more accessible.2 For traditional Medicaid enrollees, the IRA ensures that vaccine coverage is a mandatory benefit and further reduces barriers to access by eliminating cost-sharing. Ensuring equal coverage for all recommended vaccines across governmentsponsored health plans will promote public health, reduce disease burden from VPDs, and prioritize reducing racial and socioeconomic disparities compared with other sources of health insurance.
Vaccine Provisions in the IRA: Pharmacist's Role
Pharmacists play a vital role in implementing public health efforts and educating the public on important legislative changes so that patients may take advantage of these new programs in real time.25 As frontline educators, and what many people consider to be the most patient-accessible member of the health care profession, pharmacists have an enormous opportunity to communicate changes from the IRA to their patients to aid in the improvement of their overall health. Pharmacists can, and should, incorporate efforts to disseminate this information into their practice through a stepwise approach. Patients who may be impacted can be identified based on insurance type and whether they are a Medicare Part D or Medicaid enrollee. Once identified, patients may be screened for all age-appropriate vaccines and educated on the IRA policy changes that may be applicable, such as new vaccine coverage or the elimination of cost-sharing for ACIP-recommended vaccines.2 Pharmacists can then recommend a patient-specific immunization schedule or, in some settings, directly immunize.
Research has consistently demonstrated increased uptake of immunizations when a pharmacist is involved.26-28 Pharmacists can serve as champions for vaccination campaigns by advocating for vaccines, immunizing patients, or both. All 50 states, Puerto Rico, and the Districtof Columbia allow pharmacists to administer vaccines under state-by-state regulations, with some even expanding the practice by authorizing vaccine administration by pharmacy technicians.29 In turn, patients appreciate the improved access by receiving immunizations in a pharmacyenvironment compared with a physician’s office, typicallyresulting in shorter wait times and none of the additional costs associated with an office visit.30 By educating theirpatients on the provisions of the IRA, pharmacists canhave an even greater impact by increasing vaccine uptake in historically underserved groups. Increased uptake ofrecommended vaccines may directly translate into betterpatient outcomes with reduced patient morbidity and fewer overall long-term health care costs.
About the Author
Libbi Green, PharmD, is a formulary operations manager at Capital Rx in Philadelphia, Pennsylvania.
References
- FACT SHEET: The Inflation Reduction Act supports workers and families. The White House. Published August 19, 2022. Accessed June 15, 2023. https://www.whitehouse.gov/briefing-room/statementsreleases/2022/08/19/fact-sheet-the-inflation-reduction-act-supportsworkers-and-families/
- Kirchhoff S. Selected health provisions of the Inflation Reduction Act. Congress.gov. Published September 1, 2022. Accessed June 15, 2023. https://crsreports.congress.gov/product/pdf/IF/IF12203
- Summary: The Inflation Reduction Act of 2022. Senate.gov. Accessed June 15, 2023. https://www.democrats.senate.gov/
- The build back better framework. The White House. Published March 31, 2021. Accessed June 15, 2023. https://www.whitehouse.gov/build-backbetter/
- McPherson L. How “Build Back Better” started, and how it’s going: a timeline. Roll Call. Published July 21, 2022. Accessed June 22, 2023. https://rollcall.com/2022/07/21/how-build-back-better-started-and-howits-going-a-timeline/
- Medicare monthly enrollment. HHS.gov. March 2023. Updated June 28, 2023. Accessed July 14, 2023. https://catalog.data.gov/dataset/medicaremonthly-enrollment
- 2023 Medicaid & CHIP beneficiaries at a glance. Data.gov. April 2023. Accessed June 17, 2023. https://www.medicaid.gov/medicaid/quality-ofcare/downloads/beneficiary-ataglance-2023.pdf
- Rudowitz R, Drake P, Tolbert J, Damico A. How many uninsured are in the coverage gap and how many could be eligible if all states adopted the Medicaid expansion? KFF. Published March 31, 2023. Accessed June 17, 2023. https://www.kff.org/medicaid/issue-brief/how-many-uninsuredare-in-the-coverage-gap-and-how-many-could-be-eligible-if-all-statesadopted-the-medicaid-expansion/
- Sayed B, Finegold K, Ashok K, et al. Medicare Part D enrollee savings from elimination of vaccine cost-sharing. Accessed June 17, 2023. https://aspe.hhs.gov/sites/default/files/documents/329fd579ada6515d3be404f06821c361/aspe-ira-vaccine-part-d.pdf
- Quality of care vaccines. Medicaid.gov. Accessed June 17, 2023. https://www.medicaid.gov/medicaid/quality-of-care/quality-improvementinitiatives/quality-of-care-vaccines/index.html
- Medicaid eligibility. Medicaid.gov. Accessed June 17, 2023. https://www.medicaid.gov/medicaid/eligibility/index.html
- How to pay for vaccines. CDC. Updated March 31, 2017. Accessed July 17, 2023. https://www.cdc.gov/vaccines/adults/pay-for-vaccines.html
- Big changes coming to Medicare Part D plans. AARP. August 15, 2022. Accessed July 17, 2023. https://www.aarp.org/politics-society/advocacy/info-2022/medicare-part-d-changes.html
- Kolobova I, Nyaku MK, Karakusevic A, Bridge D, Fotheringham I, O’Brien M. Burden of vaccine-preventable diseases among at-risk adult populations in the US. Hum Vaccin Immunother. 2022;18(5):2054602. doi:10.1080/21645515.2022.205460
- Philip RK, Attwell K, Breuer T, Di Pasquale A, Lopalco PL. Life-course immunization as a gateway to health. Expert Rev Vaccines. 2018;17(10):851- 864. doi:10.1080/14760584.2018.1527690
- R.my V, Z.llner Y, Heckmann U. Vaccination: the cornerstone of an efficient healthcare system. J Mark Access Health Policy. 2015;3. doi:10.3402/jmahp.v3.27041
- Lu PJ, Hung MC, Srivastav A, et al. Surveillance of vaccination coverage among adult populations - United States, 2018. MMWR Surveill Summ. 2021;70(3):1-26. doi:10.15585/mmwr.ss7003a1
- Immunization and infectious diseases. HealthyPeople.gov. 2020. Accessed June 18, 2023. https://wayback.archive-it.org/5774/20220414135306/https://www.healthypeople.gov/2020/topics-objectives/topic/immunization-andinfectious-diseases/national-snapshot
- Healthy People 2030. HHS.gov. Accessed June 22, 2023. https://health.gov/healthypeople/objectives-and-data/browse-objectives/vaccination
- Vaccination coverage among adults in the United States, National Health Interview Survey, 2017. CDC. Accessed June 18, 2023. https://www.cdc.gov/vaccines/imz-managers/coverage/adultvaxview/pubs-resources/NHIS-2017.html
- Terlizzi EP, Black LI. Shingles vaccination among adults aged 60 and over: United States, 2018. CDC.gov. Published August 26, 2022. Accessed June 22, 2023. https://www.cdc.gov/nchs/products/databriefs/db370.htm
- Vogelsang EM, Polonijo AN. Scarier than the flu shot?: the social determinants of shingles and influenza vaccinations among U.S. older adults. Vaccine. 2022;40(47):6747-6755. doi:10.1016/j.vaccine.2022.09.061.
- Vaccination programs: reducing client out-of-pocket costs. The Community Guide. Updated December 23, 2015. Accessed June 17, 2023. https://www.thecommunityguide.org/findings/vaccination-programsreducing-client-out-pocket-costs.html
- Out-of-pocket costs for Medicare Part D enrollees on Part D covered vaccines. HHS.gov. Accessed June 23, 2023. https://www.hhs.gov/sites/default/files/ira-part-d-vaccines.pdf
- ASHP statement on the pharmacist’s role in public health. ASHP. Accessed June 23, 2023. https://www.ashp.org/-/media/assets/policy-guidelines/docs/statements/pharmacists-role-public-health.pdf
- Isenor JE, Edwards NT, Alia TA, et al. Impact of pharmacists as immunizers on vaccination rates: a systematic review and meta-analysis. Vaccine. 2016;34(47):5708-5723. doi:10.1016/j.vaccine.2016.08.085
- Le LM, Veettil SK, Donaldson D, et al. The impact of pharmacist involvement on immunization uptake and other outcomes: an updated systematic review and meta-analysis. J Am Pharm Assoc (2003). 2022;62(5):1499-1513.e16. doi:10.1016/j.japh.2022.06.008
- Higginbotham S, Stewart A, Pfalzgraf A. Impact of a pharmacist immunizer on adult immunization rates. J Am Pharm Assoc (2003). 2012;52(3):367-371. doi:10.1331/JAPhA.2012.10083
- Pharmacist immunization authority. NASPA. Published April 25, 2023. Accessed June 23, 2023. https://naspa.us/resource/pharmacist-authority-to-immunize/
- The essential role of community pharmacies in expanding access to vaccines. AJMC. Published July 26, 2018. Accessed June 23, 2023. https://www.ajmc.com/view/essential-role-community-pharmacies-expanding-access-vaccines

Newsletter
Stay informed on drug updates, treatment guidelines, and pharmacy practice trends—subscribe to Pharmacy Times for weekly clinical insights.





