Article
Clinical Overview: Biologic Agents for the Treatment of Crohn Disease
Author(s):
As more becomes known about Crohn disease, treatment modalities have evolved with biologic monoclonal antibodies becoming a key part of guideline- and evidence-based medicine.
Crohn disease, an autoimmune gastrointestinal disease, is 1 of 2 types of inflammatory bowel disease with possible inflammation spanning the entire thickness of the bowel wall. Crohn disease has the potential to affect the entire gastrointestinal tract from the mouth to the colon.1 Typically, in Crohn disease, there is a wide variability from patient to patient and the disease course tends to follow a relapsing and remitting pattern with overall disease progression.2
Image Credit: Adobe Stock - sdecoret

Although the etiology of Crohn disease is unknown, it is thought to be an inappropriate immune response to environmental factors within the gastrointestinal tract and it shows a bimodal distribution affecting those between 15 and 30 years of age and 40 and 60 years of age.1 As more becomes known about the disease, treatment modalities have evolved over the years with biologic monoclonal antibodies becoming a key part of guideline- and evidence-based medicine.
Currently, the American Gastroenterological Association and the American College of Gastroenterology have advocated for the use of biologic agents as mainstays of therapy with recommendations to be used for patients with moderate to severe Crohn disease.2,3 A patient is defined as having moderate to severe Crohn disease when they have a high risk of disease-related complications, including a significant impact on quality of life, inflammatory and gastrointestinal disease tract burden, hospitalization, or need for surgery.3
A patient may also be considered to have moderate to severe Crohn disease as evidenced by the gold standard scoring system of the Crohn’s Disease Activity Index (CDAI) Score that includes demographics, subjective symptoms and complaints, laboratory values, and extraintestinal findings with scores ranging from 0–600.4
For a patient to be considered to have moderate disease, a score would fall within the range of 220–450, with severe disease scoring over 450.5 Approved agents for biologic immunomodulator pharmacotherapy for moderate to severe Crohn disease includes infliximab, adalimumab, and certolizumab-pegol as first line agents. Second line agents are vedolizumab and ustekinumab, with natalizumab no longer being recommended due to the risk of progressive multifocal leukoencephalopathy.2,6
In most cases, biologic agents are initiated in the lack of response to conventional therapy options, such as corticosteroids, thiopurines, or methotrexate.1 A summary of current available biologics utilized in Crohn disease can be seen in Table 1.
Table 1. Summary of Biologics Currently Recommended for the Treatment of Crohn Disease
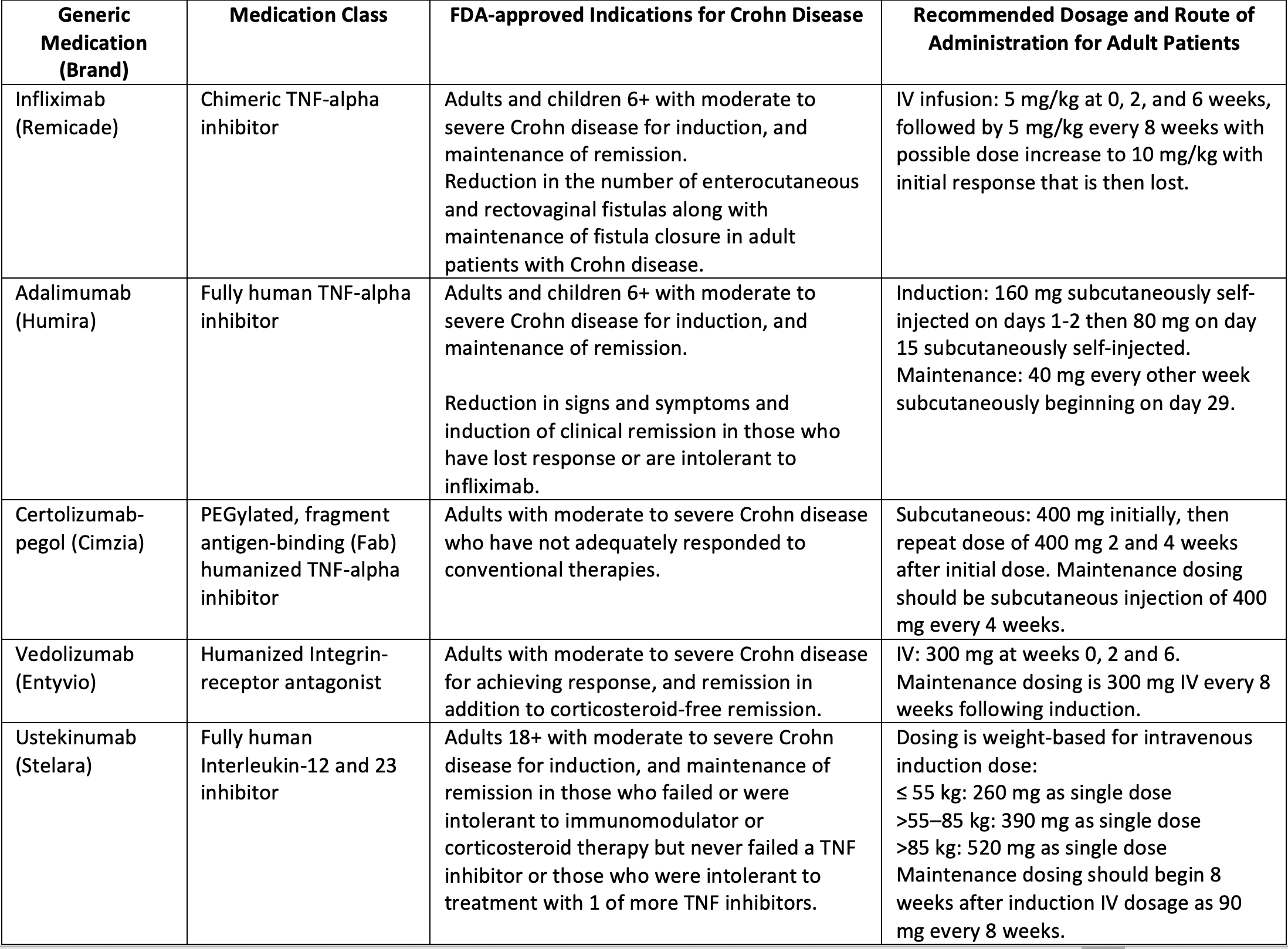
Infliximab, a chimeric TNF-alpha inhibitor, was the first monoclonal antibody to gain approval for Crohn disease therapy.6 Currently, infliximab is indicated for patients 6 years of age and older with moderately to severely active Crohn disease along with reduction and maintenance of fistulas and closure in adult patients.
The approval for Crohn disease was the result of 2 key clinical trials, the TARGAN study and the ACCENT-I randomized trial. In the 1997 TARGAN 12-week multicentered, double-blinded, randomized, controlled trial, 108 patients with moderate to severe Crohn disease resistant to conventional therapy were randomly assigned to receive either placebo or infliximab (weight-based) infusion to assess clinical response.7
In this study, clinical response was defined as an improvement of 70 points for the CDAI score. In those who received an infliximab infusion compared to placebo, an early clinical response was present in 61% and 65% of patients on infliximab at weeks 2 and 4, respectively, whereas 17% of patients receiving placebo had a clinical response at weeks 2 and 4, with the infliximab group receiving 5 mg/kg showing the highest rate of clinical response at 81%.7
Throughout the remaining 8 weeks of the trial, the differences in clinical response between the placebo and therapy groups remained significant, indicating that infliximab was beneficial for induction therapy in Crohn disease.7 Similarly, in the ACCENT-I multicentered, randomized, double-blinded trial, infliximab was compared to placebo for maintaining remission in patients with Crohn disease. In patients who received infliximab, remission rates were seen much sooner, with longer time to loss of response than patients who received placebo, supporting the use of infliximab to be used for maintenance of remission.8
Adalimumab was developed following infliximab as a fully human tumor necrosis factor blocker, with less potential to cause immunogenic adverse effects than its chimeric counterpart.6 Approved for both pediatric and adult patients with moderate to severe Crohn disease for induction and maintenance treatment, it is also indicated for patients who have not had an adequate response to infliximab due to intolerance or lack of response.3
Although multiple trials have been conducted on the use of adalimumab in Crohn disease, the CLASSIC-I trial clearly showed the benefits of induction therapy through the enrollment of 299 patients naïve to TNF blocker therapy, randomized to receive placebo or various doses of adalimumab (160 mg/80 mg vs 80 mg/40 mg vs 40 mg/20 mg).9 The CLASSIC-I trial showcased that despite similar baseline CDAI scores across all groups, patients in the adalimumab 80 mg/40 mg and 160 mg/80 mg groups had lower mean CDAI scores than patients in the placebo group beginning at week 1 of therapy.
In this placebo-controlled, multicentered, double-blinded, randomized, controlled trial, adalimumab was found to be superior to placebo in inducing remission and response in biologic-naïve patients with moderate to severe Crohn disease.9 In patients receiving adalimumab, those receiving the higher doses had greater reduction in the CDAI score as well at the 4-week mark.9
Certolizumab-pegol is another choice for a first-line option for patients who have not adequately responded to infliximab or adalimumab and who have moderate to severe Crohn disease.3 In 2 randomized, placebo-controlled, double-blinded studies in which certolizumab-pegol was administered 400 mg subcutaneously, there was a reduction in CDAI score, with patients showing a significant difference in clinical response, as defined by a reduction of CDAI score by 100, compared to placebo.10
As a humanized TNF-alpha inhibitor, certolizumab-pegol has less immunogenicity potential than infliximab but more than adalimumab. This, in addition to an indirect comparison through a meta-analysis, found certolizumab-pegol was less effective than infliximab in both induction and maintenance treatment but still a viable option.2,3
Other options for biologic therapy in the treatment of moderately to severely active Crohn disease include vedolizumab and ustekinumab, which are typically reserved as second-line agents after failure of a TNF-alpha inhibitor. Vedolizumab is a humanized integrin receptor inhibitor whereas ustekinumab is an interleukin-12 and interleukin-23 inhibitor.
Vedolizumab was studied in double-blind, randomized, placebo-controlled trials in patients with Crohn disease who had failed conventional therapy that included at least 1 TNF-alpha blocker. In these trials, unlike the previous trials, there was no significant difference found between the week 6 difference of those taking vedolizumab versus placebo despite lower CDAI scores in the active treatment group for induction.11 For maintenance, the difference was found to be significant at 52 weeks, suggesting that vedolizumab takes a longer time to remission compared to other agents.12
Ustelkimumab, similar to many of the other biologic agents, has evidence for the use of both induction and remission, but more of its long-term effect and safety profile data have been extrapolated from current available literature regarding patients with psoriasis due to the lack of long-term exposure in patients with Crohn disease.2 It is also indicated for adult patients who failed or were intolerant to immunomodulator or corticosteroid therapy despite not trying a TNF-blocker for therapy prior.2
With the development and incorporation of biologic agents into the treatment of Crohn disease, patients now have options outside of conventional therapy to help manage both induction and remission should therapy fail. Biologic treatment options offer a significant reduction in the CDAI and overall quality of life in patients with Crohn disease and as time goes on, there will hopefully be a reduction in disease complications as patients are started on therapies earlier.
References
- Ranasinghe IR, Hsu R. Crohn Disease. [Updated 2022 May 15]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK436021/
- Lichtenstein, Gary R MD, FACG1; Loftus, Edward V MD, FACG2; Isaacs, Kim L MD, PhD, FACG3; Regueiro, Miguel D MD, FACG4; Gerson, Lauren B MD, MSc, MACG (GRADE Methodologist)5,†; Sands, Bruce E MD, MS, FACG6. ACG Clinical Guideline: Management of Crohn's Disease in Adults. American Journal of Gastroenterology 113(4):p 481-517, April 2018. | DOI: 10.1038/ajg.2018.27
- Feuerstein JD, Ho EY, Shmidt E, Singh H, Falck-Ytter Y, Sultan S, Terdiman JP; American Gastroenterological Association Institute Clinical Guidelines Committee. AGA Clinical Practice Guidelines on the Medical Management of Moderate to Severe Luminal and Perianal Fistulizing Crohn's Disease. Gastroenterology. 2021 Jun;160(7):2496-2508. doi: 10.1053/j.gastro.2021.04.022. PMID: 34051983; PMCID: PMC8988893.
- McDowell C, Farooq U, Haseeb M. Inflammatory Bowel Disease. [Updated 2022 Jun 27]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK470312/
- Jesse K. Liu, Gary R. Lichtenstein,Chapter 21 - Inflammatory Bowel Disease, Editor(s): Gregory G. Ginsberg, Christopher J. Gostout, Michael L. Kochman, Ian D. Norton, Clinical Gastrointestinal Endoscopy (Second Edition), W.B. Saunders, 2012, Pages 243-264, ISBN 9781437715293, https://doi.org/10.1016/B978-1-4377-1529-3.00021-X.
- Kumar A, Cole A, Segal J, Smith P, Limdi JK. A review of the therapeutic management of Crohn's disease. Therap Adv Gastroenterol. 2022 Feb 17;15:17562848221078456. doi: 10.1177/17562848221078456. PMID: 35198041; PMCID: PMC8859667.
- Targan SR, Hanauer SB, van Deventer SJ, Mayer L, Present DH, Braakman T, DeWoody KL, Schaible TF, Rutgeerts PJ. A short-term study of chimeric monoclonal antibody cA2 to tumor necrosis factor alpha for Crohn's disease. Crohn's Disease cA2 Study Group. N Engl J Med. 1997 Oct 9;337(15):1029-35. doi: 10.1056/NEJM199710093371502. PMID: 9321530.
- Hanauer SB, Feagan BG, Lichtenstein GR, Mayer LF, Schreiber S, Colombel JF, Rachmilewitz D, Wolf DC, Olson A, Bao W, Rutgeerts P; ACCENT I Study Group. Maintenance infliximab for Crohn's disease: the ACCENT I randomised trial. Lancet. 2002 May 4;359(9317):1541-9. doi: 10.1016/S0140-6736(02)08512-4. PMID: 12047962.
- Hanauer SB, Sandborn WJ, Rutgeerts P, Fedorak RN, Lukas M, MacIntosh D, Panaccione R, Wolf D, Pollack P. Human anti-tumor necrosis factor monoclonal antibody (adalimumab) in Crohn's disease: the CLASSIC-I trial. Gastroenterology. 2006 Feb;130(2):323-33; quiz 591. doi: 10.1053/j.gastro.2005.11.030. PMID: 16472588.
- CIMZIA [package insert]. Smyrna, GA: UCB, Inc.; 2008.
- Ha C, Kornbluth A. Vedolizumab as a Treatment for Crohn's Disease and Ulcerative Colitis. Gastroenterol Hepatol (N Y). 2014 Dec;10(12):793-800. PMID: 27524947; PMCID: PMC4980813.
- ENTYVIO [package insert]. Lexington, MA: Takeda Pharmaceuticals U.S.A, Inc.; 2014.
Newsletter
Stay informed on drug updates, treatment guidelines, and pharmacy practice trends—subscribe to Pharmacy Times for weekly clinical insights.






