News
Article
Potential Host, Viral Mediators of NSV Identified, May Represent Targets to Disrupt HIV Persistence
Author(s):
Further research of these mechanisms could be significant in developing future strategies to disrupt the viral persistence in individuals living with HIV.
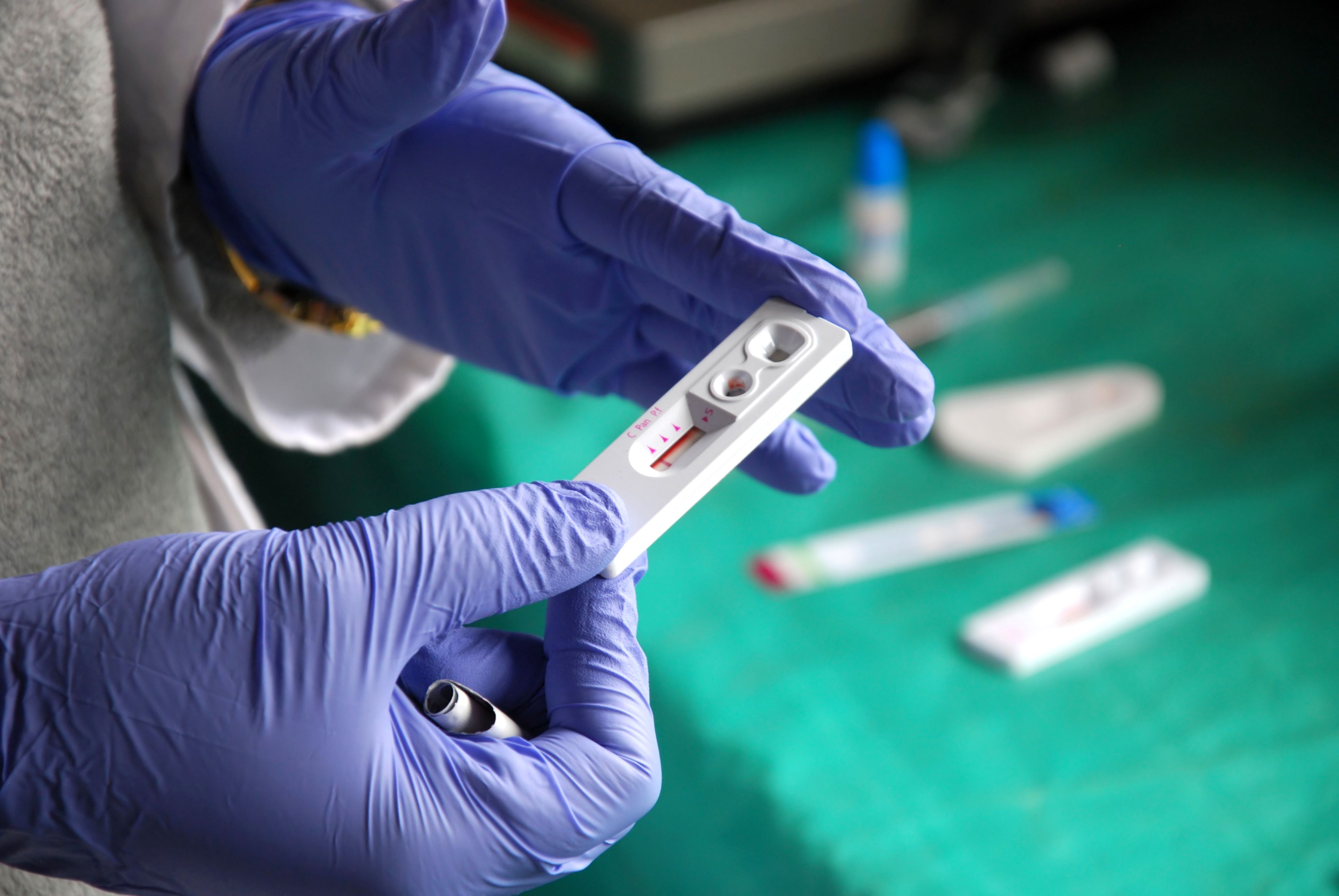
A recent study published in Nature Medicine uncovered mediators of persistent HIV viremia. HIV enters specific immune system cells and replicates inside them, and individuals with HIV are treated with antiretroviral therapy (ART) to prevent viral replication; however, some individuals on ART may continue to have low levels of viral presence in the bloodstream—viremia.1
Image credit: artegorov3@gmail | stock.adobe.com
The study recruited 8 individuals with non-suppressible HIV viremia (NSV)—a condition where low-level viremia occurs—despite receiving ART and both the virus and host immune response were examined. Patients had a median ART duration of 10 years, and the median duration of virologic suppression before NSV and the duration of NSV for the enrolled participants were 4 and 2 years, respectively. During NSV episodes, each participant received at least 2 active antiretroviral drugs.
ART adherence was assessed by the quantification of antiretroviral dug concentrations—as well as their antibodies—in plasma or through dried blood spot testing. Including the highest odds of suppression and lowest odds of future viremia, the concentrations were consistent with expected levels in ART-suppressed individuals, indicating that patients with NSV had both high levels of short-term and cumulative ART adherence.
“Our study has identified potential mediators of NSV,” said Jonathan Li, MD, Division of Infectious Diseases. “Furthering our understanding of these mechanisms could help develop strategies to disrupt viral persistence in all patients living with HIV.”
Using sequencing assessments, the investigators discovered that large reservoirs of proviruses, or viral genetic material that has been integrated into host DNA, were inserted into transcriptionally active regions of immune cell genomes. These proviruses, which were unable to replicate due to ART, contained mutations that allowed them to evade detection, expressing genes leading to the NSV phenotype.
According to the authors, the results indicate that NSV is primarily composed of 1 to 2 large plasma viral clones that are made of greater than 70% of plasma viruses. In addition, the viral clones act as the primary driver of NSV across multiple longitudinal time points; however, evidence did not confirm plasma viral sequence changes and evolution.Further, the study participants had altered gene expression patterns that contributed to a dampened immune response and increased survival of cells that were infected with HIV.
Prior research indicates that residual viremia is largely composed of drug-sensitive virus and somewhat homogeneous viral populations, and the current study authors state that it is likely mechanisms behind NSV are present in most people living with HIV contributing to low levels of residual viremia, even if ART is successful.1,2
References
1. Brigham and Women’s Hospital. Study uncovers mediators of persistent HIV viremia. News release. November 14, 2023. Accessed November 29, 2023. https://www.eurekalert.org/news-releases/1008041
2. Mohammadi, A., Etemad, B., Zhang, X. et al. Viral and host mediators of non-suppressible HIV-1 viremia. Nat Med (2023). https://doi.org/10.1038/s41591-023-02611-1
Newsletter
Stay informed on drug updates, treatment guidelines, and pharmacy practice trends—subscribe to Pharmacy Times for weekly clinical insights.
2 Commerce Drive
Cranbury, NJ 08512
All rights reserved.