Pharmacy-Led Oral Chemotherapy Management Programs
Episodes in this series

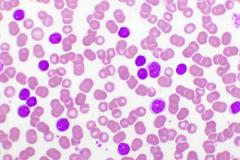
Experienced pharmacists in the management of chronic lymphocytic leukemia (CLL) discuss the impact of pharmacy-led oral chemotherapy management programs, and how they are implemented.
Cody Steeves, PharmD, BCOP: Discuss the pharmacy-led oral chemotherapy management program, if it's implemented at your institution, and how it may help adherence with that, which we have discussed a lot of adherence so far, but anything else about that. And then again touch on medication access with that.
Alison Duffy, PharmD, BCOP: At University of Maryland, pharmacists are involved in some clinics. We'd love to be in all clinics if we had enough people. We've been able to implement processes to provide initial education, ideally during that clinic encounter, and if not in clinic, having an initial follow-up call 2 to 3 days after a therapy is decided, that clinic visit when therapy is decided upon, to assess medication comprehension, retention, as well as helping with that medication access.
Either way, as pharmacists in a clinic, we're always working on how to facilitate and improve medication access initially, and then also for refills, because that timely access for CLL [chronic lymphocytic leukemia] and other leukemias, lymphomas in general, is really important.
Medication access includes discussing with the patients and pharmacies, insurance companies, and also ensuring that patients have the correct, up-to-date prescriptions. If there was a dose change, we make sure the prescription reflects that. The patient has a valid prescription, refills are sufficient. The patient knows which pharmacy to follow up with and how soon to do that. So I think the access piece is really helpful in our management programs.
Again, I think combination therapies can be extremely complicated for everybody involved, not just the patients, and it's getting more complicated with lead-in phases for different oral agents, and completely different schedules.
So part of the education should involve developing a clear communication plan for both IV [intravenous] and oral therapies. Overall, our approach to oral chemotherapy education mirrors much of the resources from the HOPA—Hematology/Oncology Pharmacy Association—website and resources and some of their checklists that I found very helpful, as well as the Oncology Nursing Society’s Oral Adherence Toolkit. Those are some of the go-to resources for those sort of education and adherence practices.
As far as adherence and toxicity assessments, for certain medications we might follow up with the patients sooner, after a week or 2. If we expect acute toxicities, for example, in a patient who's starting venetoclax outpatient, we would follow them more closely because of the risk of tumor lysis early on.
Otherwise we aim to follow patients monthly, and then we might move to every 3 months, based on determining clinical stability, which is made by the pharmacists working with the provider and nurse in that designated clinic. Also our process in implementing these management programs is a collaborative one, and so at the committee of quality improvement level at our institution, we have many of the key nurse pharmacists, providers, stakeholders, as well.
That's what we do within the clinic setting. We also work with our specialty pharmacy colleagues at our institution very closely, and certainly others at other pharmacies, depending on where the prescription needs to be filled. We're working on evaluating our programs now from a quality perspective. What has been your experience in managing these cases and following up? How does that work in your practice?
Cody Steeves, PharmD, BCOP: In specialty pharmacy we take the prescription, and it eventually gets to a pharmacist to determine clinical appropriateness and things like that, which is rarely a problem. I think, much like in a cancer, the best form of treatment is prevention in the first place.
The best way to maintain the adherence is to stress the importance of it in the initial counseling that a pharmacist would provide to a patient. That would be developing a strategy, developing a calendar, developing a time of day that's going to be best for them to take the medications. Like you mentioned, all 3 main therapies we're speaking of today have different factors that need to be considered when we develop that schedule.
But medication access, of course, any specialty pharmacy is going to work with insurance, it's going to work with access. Patient access foundations, they can provide copay assistance.
The manufacturers for commercially insured patients are almost always going to have copay cards that will take a $150 copay down to $10, or however that might work for every individual drug. We make sure we have databases full of those, ready to load them up pretty much without asking the patient, because no one's going to say no to much lower copays.
We help with that a lot, and following up. If they are filling it every 37 days, asking them why, instead of every 30 days, and keeping on track with patients as best we can to make sure we're maintaining that adherence long term with follow-ups with clinical staff, and making sure the prescriptions are coming in.
If they have a change in dose, we ask them why. Was it because of an adverse effect? Was it because of something we could have prevented, possibly? Or is it because you're taking a new medicine that you need or don't need? We try to make sure we're staying on top of everything from that angle as well, as a pharmacy and as pharmacists.
Alison Duffy, PharmD, BCOP: It's interesting to share both of our experiences because it highlights that there are so many people involved in each patient's care who can be so helpful in the education.
It'll be important to see, as some of the practices evolve, if we can improve the communication between all those involved so that we're working together. And that everybody is aware of the clear treatment plan for the patient and if that changes, so everybody can be successful in educating the patient, and detecting interactions, and helping with adherence.
How exactly do we do that across the board without an integrated system, so everybody is seeing the same information? It's really hard.
I think communication is key here, and realizing that we're all colleagues who are working together for the same purpose. That's so much easier when everybody has the same information about that patient, including that patient, because obviously that could be really confusing if they're getting lots of different information. I think that's great.