Burden and Disease Characteristics of Melanoma
Episodes in this series
In this Pharmacy Times program for Health Systems Pharmacists, Nanaz Amini, PharmD, RPh, MS, of the Angles Clinic, provides a pharmacist’s perspective on the management of melanoma.
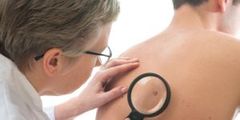
TranscriptNanaz Amini, PharmD, RPh, MS: It really depends age-wise. Basically, this melanoma is the second in line for life years lost for our patients that are in their 20s and 30s. It seems that the younger the patients are, the burden of loss is a lot more, obviously. And their prognosis when you have melanoma at a younger age is very grim. In addition to that, just a statistical fact, 1 person dies of melanoma every hour, which that is something that, growing up, smoking was always associated with how many people are dying. You never thought a skin cancer is definitely melanoma, that there was such high prevalence of it, but there is. They project that in just this year, there will be about 9700 patients that will be diagnosed with melanoma. So, the burden is quite high just because of, I think, more screening, more vigilance, and more exposure—people knowing of melanoma and cancers, so you’re seeing it more, and knowing people died of a melanoma and the years lost from it.
Obviously, the staging of melanoma is you have stage 0, which is really nothing, and stage 1 through 4. And the for prognosis, patients who are in stage 1 usually have about a 5-year survival rate of 95%. And as the staging goes higher—obviously there, it’s multifaceted—definitely the survival rate is lower. If patients have stage 2, depending on involvement of ulceration and whatnot, it will go down anywhere in the 70 percentile. Patients who have nodal involvement, which are patients who are in stage 3, it can go down anywhere from 50% to 35% or even 25%. In patients with stage 4, it is definitely closer to like 19% and below. So, obviously, it correlates. As the stage is higher, the burden of it, and prognosis, is worse. And all these prognoses are like 5 years of survival rates, based on the staging.
It depends really also age-wise. Because when you have patients that are younger, they may just have a mole, which is a stage 1. It may be removed and there’s no reoccurrence, but it depends on if it’s ulcerated or not, and that can increase within 1 year. There are patients who are diagnosed, but they are not diagnosed until they have like a stage 3. So, that prognosis is very grim in the sense of going from stage 3 to stage 4. It may take not a lot of time. It also depends on the kind of melanoma they have.
There’s also genetic profiling that’s done, and those factors do help in therapies that are available in how long those therapies are durable for and if they can move up staging. But there are patients who from the aggressiveness of their individual disease, it could be a year. But there are patients that we have that have survived melanoma. They were stage 3, stage 4, and they’re not disease-free, but they have stable disease for the past 4 or 5 years. Therefore, it really depends when they were diagnosed with melanoma.
So, patients that were diagnosed 10 years ago—and there were minimal therapies available—they went from one stage to the next within no amount of time. Now based on the fact that we have all these new therapies, we are delaying that process. It really depends on the patient population, you’re looking at the age of the patients, how aggressive their particular disease is, and, also, when they were diagnosed with melanoma and what therapies are available at that particular time. It is hard to say, from stage 1 to 2, how long it would take. Usually, from stage 1, you’re not necessarily going to go to stage 2 because the survival rate is very good—it’s 95% to 98%. And it may never reoccur. Patients who are stage 2, do have ulcerations, and may have some complications, it really depends. But patients with stage 3 and 4, it could be months, it could be years. It really depends.
It has significantly changed the paradigm because before you had dacarbazine, you had a handful of drugs that worked for melanoma. But, really, there was no long-term benefit, people were not surviving. There is a survival rate now with immunotherapy, overall survivals with things like Yervoy (ipilimumab), that have come. That was the first in 2010, followed with Keytruda (pembrolizumab), and followed with Opdivo (nivolumab). All of those medications now—and they’re all immunotherapies—have changed the paradigm completely because those are first in line that are used, as opposed to the chemotherapies that were originally the only thing available for patients who had melanoma. There’s a complete shift in how patients are treated. So, first in line would be the immunotherapies as opposed to the old dacarbazines and things of that nature, which were quite harsh on patients, too, not just durable response. And their rates, overall survival, progression-free survival, have significantly changed from having immunotherapy available for patients.