Précis
Through recognizing the importance of research in the scope of pharmacy practice by national pharmacy organizations, research can become a prominent role and responsibility of pharmacy.
Introduction
Scholarship in Oncology Pharmacy Practice
About the Authors
Ryan Beechinor, PharmD, BCPS, BCOP, is a senior pharmacist at the University of California (UC), Davis Comprehensive Cancer Center and an assistant professor at the University of California, San Francisco School of Pharmacy.
Cody Angerman, PharmD, is a PGY2 oncology resident at the UC Davis Medical Center in Sacramento, California.
Aaron Steele, PharmD, BCOP, is a senior pharmacist in the Department of Pharmacy at the UC Davis Medical Center in Sacramento, California.
In 2016, the American College of Clinical Pharmacy Board of Regents published a white paper titled “The Importance of Research and Scholarly Activity in Pharmacy Training.” It highlighted the importance of pharmacist-led research and described some barriers to engaging in high-quality, impactful research that pharmacists face.1 Currently, most first postgraduate year (PGY1) or second postgraduate year (PGY2) residency programs rely on retrospective designs for their residency projects. However, current residency project publication rates are dismal, with estimates of successful publication between 1.8% and 4.3%.2,3 This is compounded by results from Stranges et al, who found that residents who publish their PGY1 or PGY2 research project are twice as likely to continue to publish within 5 years after residency as those who do not publish their research projects.4 Therefore, to get more pharmacists involved in peer-reviewed publications, it is important that the design and/or content of their research be publishable. However, it is vital that the importance of research be recognized in the scope of pharmacy practice by national pharmacy organizations, which can facilitate incorporation of research among prominent roles and responsibilities of pharmacy.
The scope of practice for hematology/oncology pharmacists, published by the Hematology/Oncology Pharmacy Association, calls on pharmacists to “contribute to cancer research by leading clinical studies, reporting important observations from practice, and supporting investigational drug service programs.”5 This has been reinforced by other reviews highlighting the unique role pharmacists play in patient care; these reviews emphasized the need for oncology pharmacist participation in clinical research efforts.6 Data on rates of publication success from hematology/oncology abstracts presented at major pharmacy meetings are more encouraging at 17.5%, but this is far from satisfactory.7 In this paper, we describe a successful pharmacy-led research project and highlight the factors that made this project publishable.
Identifying an Environment for a Publishable Research Project
One of the ways to ensure a pharmacy-led research project is publishable is to base the project on a change that happens in clinical practice.1,8,9 This can be a new drug approval, indication, or administration method. A project becomes more valid and thus more likely to be published when it creates a dynamic whereby different institutions have different practices about use. In the project that we will describe, the research question benefited from having both of these factors: A new administration method was made available, which led to heterogeneity in practices across cancer centers.
In 2015, the intravenous (IV) formulation of daratumumab (Darzalex; Janssen Biotech) became the first FDA-approved anti-CD38 antibody for use in patients with previously treated multiple myeloma.8 In 2019, based on the results of the phase 3 CASSIOPEIA (NCT02541383) and MAIA (NCT02252172) trials, it received FDA approval for newly diagnosed multiple myeloma in the transplant-eligible and transplant-ineligible populations.9 However, due to the relatively high frequency of infusion-related reactions (IRRs) following IV administration of daratumumab in the phase 2 data, most of the phase 3 protocols utilized a 6-hour observation time post infusion.10 Additionally, long observation times led to increased burden of resources for chair times, patient admittance to the hospital to finish the infusion, creative strategies such as splitting the dose over 2 days, and subsequent decreased patient satisfaction.
The manufacturer of daratumumab, Janssen Biotech, having observed the incidence of IRRs with IV daratumumab, in 2016 began engaging with the FDA to develop a formulation of the agent combined with recombinant human hyaluronidase for subcutaneous injection.11 This led to the FDA approval of daratumumab and hyaluronidase-fihj (Darzalex Faspro; Janssen Biotech) in 2020, based on the results of the phase 3 COLUMBA (NCT03277105) trial.12 Although the trial showed a lower incidence of IRRs compared with the IV formulation of daratumumab, the supplementary appendix indicated that investigators still used a 6-hour observation time after the first dose and as deemed necessary by the investigator for subsequent injections (although, notably, this was absent from the prescribing information).12,13 However, the lack of clarity in terms of observation times with the use of subcutaneous daratumumab led to differing institutional standards, with some centers recommending a 4-hour observation and some only 1 hour.14,15 This led to several retrospective analyses, which aimed to shorten the duration of observation time.16-18
Identifying an Intervention for a Publishable Research Project
Most retrospective research projects have a disease state end point (eg, efficacy and/or safety). Retrospective studies are fraught with confounding bias, mostly stemming from their nonrandomized nature, which leads to a lack of generalizability. A third strategy that can increase the chance of pharmacy-led research being published is to focus the intervention on something more patient focused. This way, if the interaction leads to better quality of life for the patient (eg, cost and/or time saved), this will be generalizable to the entire population of patients with cancer. We have provided 4 examples of such interventions below:
- An intervention that optimizes the amount of time a patient spends in their home (eg, a regimen typically given in the inpatient setting, testing whether it can be given in the outpatient setting with similar efficacy/safety).
- An intervention that improves the time required for treatment (eg, testing rapid infusions of anticancer medications, which can reduce chair time).
- An intervention that seeks to ease the burden of caregivers and/or families. The current body of literature in oncology inadequately addresses these profound aspects, despite the well-established understanding of the psychosocial and emotional effects on caregiver experiences.
- An intervention aimed at remotely monitoring and managing common symptoms experienced by patients with cancer, such as pain, nausea, and fatigue. This intervention aims to reduce unnecessary clinic visits, improve symptom control, and enhance overall patient well-being.
An Example From the Literature
In 2023, Maples et al published a seminal paper about optimization of daratumumab administration, “Eliminating the Monitoring Period With Subcutaneous Daratumumab: A Single-Center Experience,” in Blood Cancer Journal.19 The authors described a 2-step process by which they first used a 2-hour observation period for the first 29 patients and reported that the IRR rate was less than 10%. They went on to remove the observation period for 35 patients; results showed that no serious IRR occurred in the zero-hour observation period group and no patients required hospitalization. Only 1 patient reported an injection site reaction (not an IRR) in this group. Authors concluded that patients can safely receive subcutaneous daratumumab without an observation period, as this contributes toward cost savings and increased infusion bed availability.19
Implementing the Results at UC Davis Health
Based on the report of Maples et al, UC Davis, as well as the other health system campuses UC-wide, has adapted practices to a zero-hour observation period for subcutaneous daratumumab starting with cycle 1. We estimate that removing the minimum mandatory observation time of 4 hours per patient, as was shown in Maples et al, and treating approximately 60 new patients annually will save more than 240 hours of observation time. Based on our internal analysis of the costs associated with observation time, we estimate this will save our health system $225,000 per year. These savings can be reallocated into chair time for other patients.
In line with the report by Maples et al, implementation of a zero-hour observation period likely has led to increased patient satisfaction through expedited discharge, as well as increased revenue through scheduling other medications in place of the observation time. Importantly, this does not apply to the IV formulation of daratumumab, which still requires observation post administration.
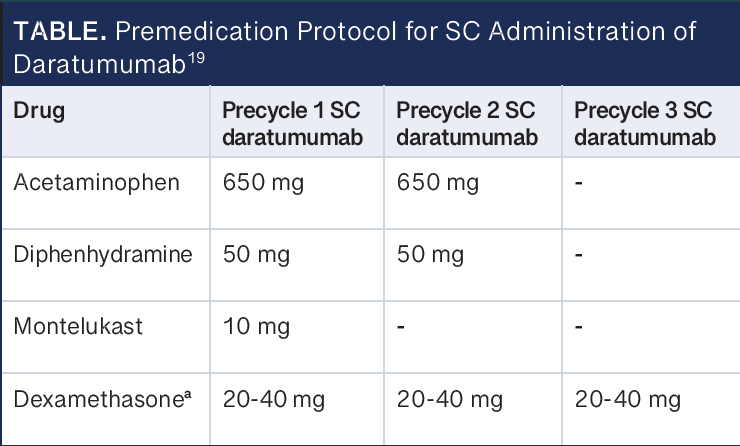
Additionally, it is still necessary to follow the premedication protocol for subcutaneous daratumumab that Maples et al utilized (Table).19 For those working at a health system that has not implemented the zero-hour observation period for subcutaneous daratumumab, it may be beneficial to consider the potential cost- and time-saving benefits and review the publication by Maples et al.19
Conclusions
We should strive to design our pharmacy projects to be more publishable using the 3 criteria captured by Maples et al: identifying a project based on a practice change, generating a research question based on variation in clinical practice, and studying an intervention that is patient focused and applicable to many centers. These factors will have a positive influence on not only the research project’s being publishable but also the project’s overall impact. With this emphasis, residency research projects have the potential to change practice while providing an invaluable opportunity for pharmacists to actively contribute to the advancement of the profession.
References
Deal EN, Stranges PM, Maxwell WD, et al; American College of Clinical Pharmacy. The importance of research and scholarly activity in pharmacy training. Pharmacotherapy. 2016;36(12):e200-e205. doi:10.1002/phar.1864
Weathers T, Ercek K, Unni EJ. PGY1 resident research projects: publication rates, project completion policies, perceived values, and barriers. Curr Pharm Teach Learn. 2019;11(6):547-556. doi:10.1016/j.cptl.2019.02.017
O’Dell KM, Shah SA. Evaluation of pharmacy practice residents’ research abstracts and publication rate. J Am Pharm Assoc (2003). 2012;52(4):524-527. doi:10.1331/JAPhA.2012.10224
Stranges PM, Vouri SM. Impact of resident research publication on early-career publication success. Am J Health Syst Pharm. 2016;73(12):895-900. doi:10.2146/ajhp150567
Scope of Hematology/Oncology Pharmacy Practice. Hematology/Oncology Pharmacy Association. 2013. Accessed March 11, 2024. https://www.hoparx.org/documents/111/HOPA13_ScopeofPracticeBk1.pdf
Holle LM, Boehnke Michaud L. Oncology pharmacists in health care delivery: vital members of the cancer care team. J Oncol Pract. 2014;10(3):e142-e145. doi:10.1200/JOP.2013.001257
Wooten KM, Arnall JR, Bowser KM, et al. Publication rates of hematology/oncology abstracts presented at major pharmacy association meetings. J Oncol Pharm Pract. Published online March 27, 2021. doi:10.1177/10781552211004700
Sanchez L, Wang Y, Siegel DS, Wang ML. Daratumumab: a first-in-class CD38 monoclonal antibody for the treatment of multiple myeloma. J Hematol Oncol. 2016;9(1):51. doi:10.1186/s13045-016-0283-0
Darzalex (daratumumab) injection. Prescribing information. Janssen Biotech Inc; 2023. Accessed March 14, 2024. https://www.janssenlabels.com/package-insert/product-monograph/prescribing-information/DARZALEX-pi.pdf
Darzalex Faspro: postinjection observation time. Janssen Scientific Affairs. Updated March 5, 2024. Accessed March 11, 2024. https://www.janssenscience.com/products/darzalex-faspro/medical-content/darzalex-faspro-postinjection-observation-time
BLA multidisciplinary review and evaluation: BLA 761145, Darzalex Faspro (daratumumab and hyaluronidase-fihj). Center for Drug Evaluation and Research. April 12, 2020. Accessed March 11, 2024. https://www.accessdata.fda.gov/drugsatfda_docs/nda/2020/761145Orig1s000MultidisciplineR.pdf
Darzalex Faspro (daratumumab/hyaluronidase). Prescribing information. Janssen Biotech; 2022. Accessed March 14, 2024. https://www.janssenlabels.com/package-insert/product-monograph/prescribing-information/DARZALEX+Faspro-pi.pdf
Mateos MV, Nahi H, Legiec W, et al. Subcutaneous versus intravenous daratumumab in patients with relapsed or refractory multiple myeloma (COLUMBA): a multicentre, open-label, non-inferiority, randomised, phase 3 trial. Lancet Haematol. 2020;7(5):e370-e380. doi:10.1016/S2352-3026(20)30070-3
Kim EB, O’Donnell E, Branagan AR, et al. Real-world observations and practical considerations of subcutaneous daratumumab administration in multiple myeloma. Blood. 2021;138(suppl 1):5018. doi:10.1182/blood-2021-153751
Kye J, Patel S, Seyer M, et al. Safety of SC daratumumab in the treatment of plasma-cell disorders: a single-center experience. J Hematol Oncol Pharm. 2023;13(2):1-6.
Davis JA, Youngberg H, Gaffney K, Duco M, Hashmi H. “Fast but not so furious”: short observation time after subcutaneous daratumumab administration is both a safe and cost-effective strategy. Clin Lymphoma Myeloma Leuk. 2022;22(8):e680-e684. doi:10.1016/j.clml.2022.03.006
Hughes DM, Henshaw L, Blevins F, et al. Standard 30-minute monitoring time and less intensive pre-medications is safe in patients treated with subcutaneous daratumumab for multiple myeloma and light chain amyloidosis. Clin Lymphoma Myeloma Leuk. 2022;22(8):566-568. doi:10.1016/j.clml.2022.03.003
Soefje SA, Carpenter C, Carlson K, et al. Clinical administration characteristics of subcutaneous and intravenous administration of daratumumab in patients with multiple myeloma at Mayo Clinic infusion centers. JCO Oncol Pract. 2023;19(4):e542-e549. doi:10.1200/OP.22.00421
Maples KT, Hall KH, Joseph NS, et al. Eliminating the monitoring period with subcutaneous daratumumab: a single-center experience. Blood Cancer J. 2023;13(1):29. doi:10.1038/s41408-023-00801-1
Disclosures
Ryan Beechinor, PharmD, BCPS, BCOP, reports having received funding/compensation for consulting and/or research activities from the following entities that are unrelated to this content: AbbVie, Aptitude Health, Children’s Oncology Group, The Dedham Group, Eunice Kennedy Shriver National Institute of Child Health and Human Development, IQVIA, Melinta Therapeutics, National Institutes of Health, Oncology Reimbursement Management, Pfizer, and Trinity Life Sciences. All remaining authors report no conflicts of interest.