Precision oncology, a cornerstone of contemporary cancer treatment, represents a shift from traditional methods of cancer treatment. This field utilizes deep understanding of the genetic and molecular makeup of cancer cells, tailoring treatments to specific genetic mutations and alterations.1 Such an approach enhances treatment efficacy by targeting the unique genetic profiles of tumors and aims to minimize adverse effects (AEs), surpassing conventional broad-spectrum therapies.2
Central to precision oncology are biomarkers, which serve as indicators of the molecular changes within tumors. They guide oncologists in selecting therapies that are likely to be effective and minimize AEs. This personalized strategy, based on predicting patient responses to specific therapies while considering unique genomic and molecular markers, results in more effective treatments with better outcomes.2
A New Era in Cancer Treatment for Pharmacy
For pharmacists, precision oncology represents a significant evolution in therapeutic practices. The rise of targeted therapies and immunotherapies has expanded treatment options, necessitating an in-depth understanding of these novel modalities. Moreover, the approach extends to early detection and prevention, identifying individuals at higher risk of developing certain cancers based on genetic predispositions.2
In the context of the most prevalent cancers in the United States, namely, breast, prostate, and lung cancer, precision oncology has achieved notable advances. Lung cancer, the most common cancer globally, benefits from an integrative approach combining genomic, transcriptomic, and proteomic data with clinical and lifestyle factors, leading to precise, individualized treatment.3 Similarly, prostate cancer, often asymptomatic in early stages, significantly benefits from precision oncology, allowing for more nuanced therapeutic strategies in consideration of the nature of the disease.4
Role of Biomarkers and Pharmacogenomics
Key to precision oncology are biomarkers, which provide insights into the genetic alterations or molecular profiles within a tumor. These biomarkers are categorized into DNA biomarkers, DNA tumor biomarkers, and general biomarkers. DNA biomarkers, such as single nucleotide polymorphisms, are essential for identifying genetic variations in patients. DNA tumor biomarkers, specific to certain cancer types, play a critical role in early detection and in the selection of effective therapies.5 General biomarkers, while broader, are useful in predicting treatment outcomes.
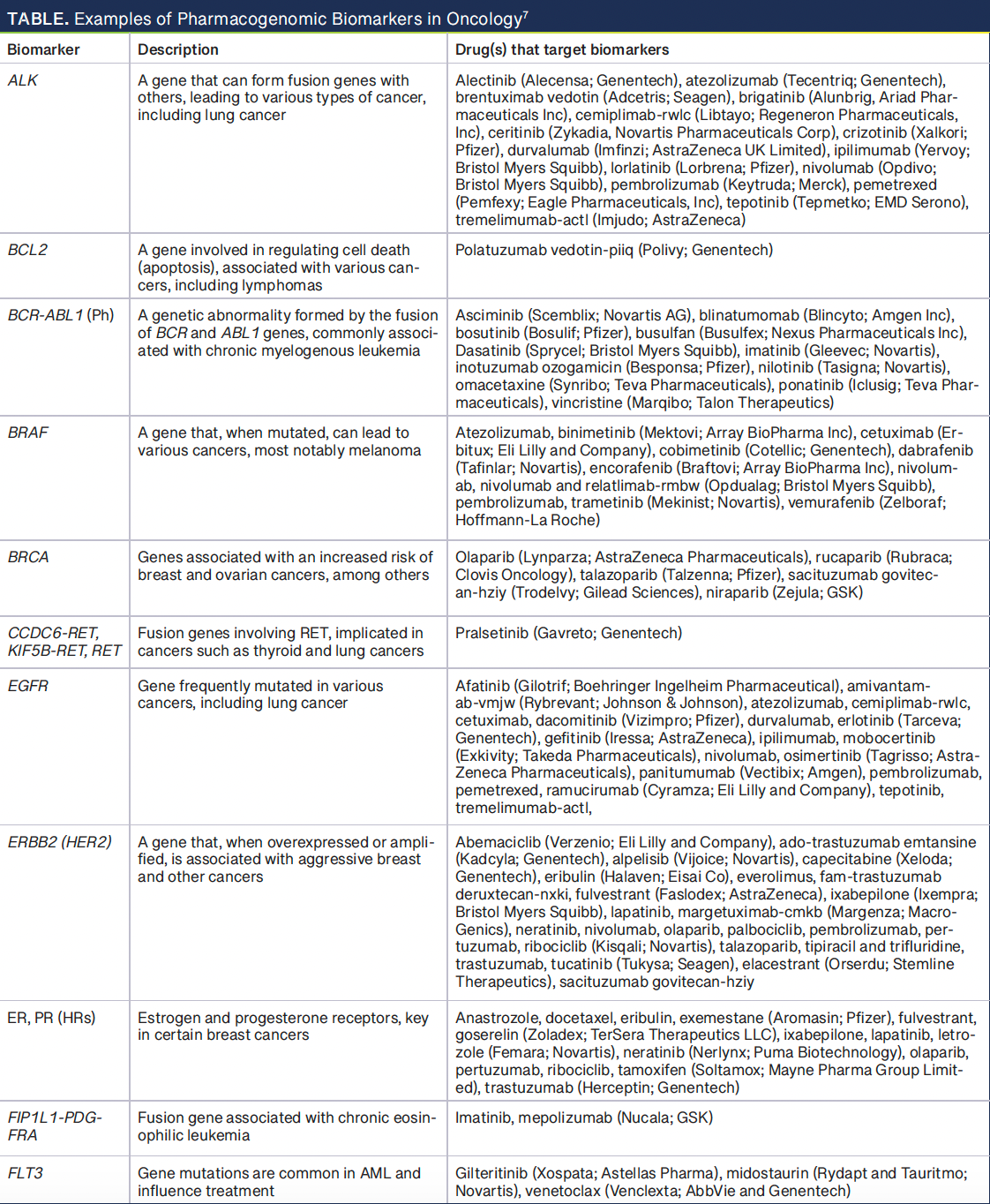
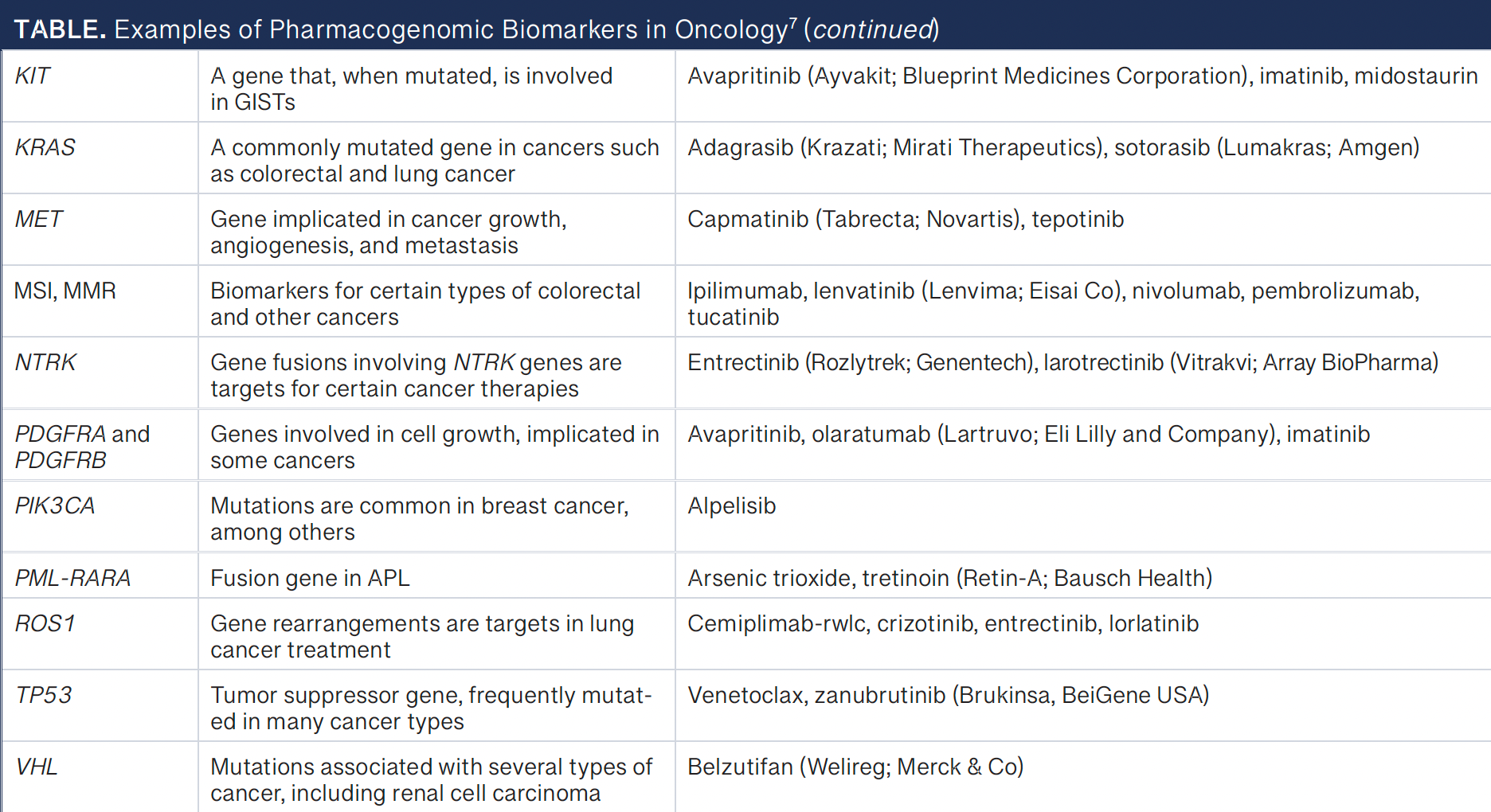
Pharmacogenomics, the study of how genetics affects drug response, is increasinglyrecognized for its role in cancer treatment. The FDA’s inclusion of pharmacogenomics information in the labeling of over 120 drugs reflects its significance in enhancing the safety and efficacy of cancer treatments.6 This field helps identify patients at risk of severe AEs and helps pharmacists tailor treatments to minimize adverse reactions. The labeling of many FDA-approved anticancer drugs with pharmacogenomics information underscores the growing importance of this approach. The table describes examples of oncology biomarkers in product labeling.7
Impact on Drug Development
Pharmacogenomics research in drug development optimizes clinical trial costs and efficiency. It aids in identifying new drug targets or pathways, enriching the understanding of drug mechanisms. The development of imatinib (Gleevec; Novartis), a targeted therapy for chronic myelocytic leukemia (CML), serves as a prime example of how pharmacogenomics research can enrich drug development. Imatinib’s development required a deep understanding of the genetic basis of CML, which involves a specific chromosomal abnormality known as the Philadelphia chromosome.6
Breast Cancer: Tailoring Treatment to Genetic Profiles
Breast cancer, the most common cancer among women worldwide, exhibits diverse subtypes and genetic markers. It is classified into groups such as estrogen receptor (ER) positive, progesterone receptor (PR) positive, HER2 positive (HER2+), and triple-negative breast cancer (TNBC), each with distinct characteristics and treatment responses.8
Subtypes and Targeted Therapies
- Luminal A tumors: Characterized by ER and/or PR presence and low Ki-67 expression. They respond well to hormone therapies such as tamoxifen (Soltamox; Mayne Pharma Group Limited), often with minimal need for chemotherapy.8
- Luminal B tumors: While ER positive, these may lack PR and have higher Ki-67 levels, indicative of a more aggressive nature. Treatment combines hormonal therapy and chemotherapy.8
- HER2+ subgroup: Known for high HER2 expression without ER and PR. Targeted therapies against HER2/neu protein, coupled with surgery and chemotherapy, have improved outcomes for this group.8
- TNBC: Lacks ER, PR, and HER2 expression, subdivided into several subgroups. TNBC is more challenging to treat due to the absence of these markers.8
Targeted therapies play a crucial role in breast cancer treatment, focusing on specific molecular pathways and cell behaviors. Current effective treatments include drugs such as everolimus (Afinitor; Novartis), bevacizumab (Avastin; Genentech), trastuzumab (Herceptin; Genentech), T-DM1 (Kadcyla; Genentech), pertuzumab (Perjeta; Genentech), and lapatinib (Tykerb; GSK), each targeting different pathways.9
The shift toward including pharmacists on the oncology care team reflects a broader approach to cancer management. Pharmacists’ involvement in both secondary and primary care settings is pivotal for patient support, ensuring optimal care and adherence to treatment regimens.10
Prostate Cancer: Advances in Personalized Care
Prostate cancer risk is influenced by age, ethnicity, family history, and specific genetic mutations. Key genes linked to increased risk include BRCA1, BRCA2, and HOXB13, and mismatch repair (MMR) genes, known for their roles in DNA repair and tumor suppression, contribute to a modest to moderate lifetime prostate cancer risk.11
Genetic Markers and Targeted Therapies
The development of prostate cancer involves somatic alterations specific to prostate cells. These mutations, including structural changes in chromosomes, significantly impact cancer progression. Targeted therapies such as talazoparib (Talzenna; Pfizer), a PARP inhibitor, and enzalutamide (Xtandi; Pfizer and Astellas), an androgen receptor inhibitor, have been approved for homologous recombination repair gene–mutated, castration-resistant prostate cancer, targeting BRCA1 and BRCA2 mutations.12
Pharmacists play a vital role in the management of prostate cancer treatments. Their involvement is crucial in ensuring treatment adherence and managing AEs. Pharmacists also regularly monitor treatment response and collaborate with health care professionals to adjust therapy as needed, significantly enhancing patient care and outcomes in prostate cancer treatment.13
Lung Cancer: From Broad Treatment to Individualized Approaches
Lung cancer’s complexity and variability demand a shift from traditional, broad treatment methods to more personalized, precision-based approaches. Advances in molecular biology and genetic profiling have revealed the diverse genetic alterations that drive lung cancer growth, leading to the development of targeted therapies. These therapies are designed to specifically address the unique molecular abnormalities in an individual’s cancer cells, improving treatment efficacy and reducing the AEs associated with more generalized treatments.14
Breakthroughs in Targeted Therapies and Immunotherapies
The landscape of lung cancer treatment has been revolutionized by the advent of targeted therapies and immunotherapies. Targeted therapies, such as tyrosine kinase inhibitors, focus on specific molecules or pathways involved in cancer progression, tailoring treatments to the genetic profile of the tumor.15,16 Immunotherapies, including therapeutic vaccines, immunomodulators, autologous cellular therapies, and monoclonal antibodies, harness the body’s immune system to recognize and eliminate cancer cells, showing promising results in certain lung cancer subtypes.17
Impact on Patient Outcomes
These advancements in lung cancer treatment have significantly improved patient outcomes, leading to better response rates and prolonged survival. Patients benefit from more effective therapies that specifically target cancer cells while minimizing damage to healthy tissues, enhancing their quality of life. The shift from broad treatment strategies to personalized approaches marks a substantial advancement in lung cancer management. The introduction of targeted therapies and immunotherapies has transformed lung cancer care, demonstrating remarkable efficacy and offering new hope to patients. With pharmacists actively involved in patient-centered care, their contributions, alongside medical advancements, continue to improve treatment outcomes, fostering optimism in the fight against lung cancer.
Challenges and Considerations in Precision Oncology
Precision oncology, although an advancement in cancer care for patients, can also present ethical, socioeconomic, and educational challenges that require careful consideration.
Ethical and Socioeconomic Factors
Precision medicine raises ethical concerns such as privacy protection, especially with genetic data. Inappropriate disclosure of sensitive information can lead to embarrassment, discrimination, and delayed health care–seeking behaviors by patients due to stigma concerns. Additionally, there are risks of genetic discrimination in employment and insurance options based on subtle genomic variations, which can have significant economic impacts.18
Equity in access to personalized medicine is another critical ethical issue. The risk of exacerbating health disparities is significant, as advanced therapies may not be equally accessible to all, favoring those with greater financial resources. Ensuring fairness and equity in access to these treatments is essential.
Cost and Accessibility of New Treatments
The cost of new cancer treatments, such as stem cell therapy, targeted therapy, and gene therapy, can be substantial, affecting their accessibility. These costs can pose financial burdens on patients and health care systems, influencing treatment choices and availability.19,20
Continuous Education for Pharmacists
In the evolving field of precision oncology, continuous education for pharmacists is crucial. Pharmacists need to be knowledgeable about personalized treatment plans, medication regimens, and the latest developments in precision medicine. Their role extends to patient education and counseling, addressing the complexities of treatments in precision oncology. Awareness of regulatory changes, reimbursement policies, and guideline updates is also vital for pharmacists in delivering effective precision oncology services.21
The Future of Cancer Treatment: What Pharmacists Need to Know
The future of cancer treatment, particularly in precision oncology, is shaped by ongoing research and the evolving role of pharmacists in cancer care teams.
Ongoing Research in Precision Oncology
Advancements in genetic profiling are crucial for the precise characterization of cancers, with an increasing focus on identifying a wider range of biomarkers and targeted therapies. Understanding the malfunctioning genes in various cancers is key to developing effective treatments. Research on drug development targets is also expanding, as evidenced by initiatives such as the Illuminating the Druggable Genome initiative, which reveals that many human proteins and potential drug targets remain understudied.22,23
Expanding Role of Pharmacists
Pharmacists are integral to multidisciplinary cancer care teams, contributing to increased adherence rates, therapy optimization, safety improvements, and cost-saving benefit.24 The role of pharmacists in cancer care is increasingly personalized, shifting from traditional tasks such as safety checks in dispensing medications to providing direct patient care at the bedside or in clinics.
Personalized Patient Care and Counseling
As precision oncology progresses, pharmacists are focusing more on personalizing treatment for patients, aiming to specify exactly what each patient needs while reducing unnecessary treatments. Pharmacists also face the challenge of staying updated with new medications in oncology, learning about their AE profiles, and counseling patients on management strategies.
Conclusion
In this era of personalized cancer treatment, pharmacists play a crucial role. Their responsibilities go beyond traditional medication dispensing, encompassing pharmacokinetics, pharmacodynamics, and clinical pharmacology. They are pivotal in providing recommendations for pharmacogenetic testing, interpreting results, and formulating patient-specific drug regimens. Furthermore, pharmacists engage in patient education, especially in areas such as direct-to-consumer genetic testing and the application of clinical pharmacogenomics.25
As the field of precision oncology evolves, continuous learning and adaptation are essential for health care professionals. Staying informed about the latest developments in genomics, targeted therapies, and new technologies is crucial. Engagement in ongoing education, through conferences, workshops, seminars, and online resources, is necessary for keeping abreast of emerging research and innovative therapies. Collaboration with experts in the field further enhances the understanding and application of precision oncology.
About the Authors
Elena Berumen is a class of 2025 PharmD candidate in the Department of Pharmacy Practice, Irma Lerma Rangel School of Pharmacy, Texas A&M University in Kingsville.
Omolara Falade is a class of 2025 PharmD candidate in the Department of Pharmacy Practice, Irma Lerma Rangel School of Pharmacy, Texas A&M University, and an MBA candidate at Texas A&M University in Kingsville.
Lanam Millican is a class of 2026 PharmD candidate in the Department of Pharmacy Practice, Irma Lerma Rangel School of Pharmacy, Texas A&M University in Kingsville.
Janet John is a class of 2027 PharmD candidatein the Department of Pharmacy Practice, Irma Lerma Rangel School of Pharmacy, Texas A&M University in Kingsville.
Alexander Adeoye is a class of 2025 PharmD candidate in the Department of Pharmacy Practice, Irma Lerma Rangel School of Pharmacy, Texas A&M University in Kingsville.
Sara Rogers, PharmD, BCPS, is a clinical assistant professor of precision medicine and ambulatory care at Irma Lerma Rangel College of Pharmacy, Texas A&M University in Kingsville; a clinical specialist at Texas A&M Physicians Clinic; and a cofounder of the American Society of Pharmacovigilance in Houston, Texas.
References
- Fountzilas E, Tsimberidou AM. Overview of precision oncology trials: challenges and opportunities. Expert Rev Clin Pharmacol. 2018;11(8):797-804. doi:10.1080/17512433.2018.1504677
- Ho D, Quake SR, McCabe ERB, et al. Enabling technologies for personalized and precision medicine. Trends Biotechnol. 2020;38(5):497-518. doi:10.1016/j.tibtech.2019.12.021
- Guan X, Qin T, Qi T. Precision medicine in lung cancer theranostics: paving the way from traditional technology to advance era. Cancer Control. 2022;29:10732748221077351. doi:10.1177/10732748221077351
- Rawla P. Epidemiology of prostate cancer. World J Oncol. 2019;10(2):63-89. doi:10.14740/wjon1191
- Song IW, Vo HH, Chen YS, et al. Precision oncology: evolving clinical trials across tumor types. Cancers (Basel). 2023;15(7):1967. doi:10.3390/cancers15071967
- Weng L, Zhang L, Peng Y, Huang RS. Pharmacogenetics and pharmacogenomics: a bridge to individualized cancer therapy. Pharmacogenomics. 2013;14(3):315-324. doi:10.2217/pgs.12.213
- Table of pharmacogenomic biomarkers in drug labeling. FDA. August 10, 2023. Accessed January 4, 2024. https://www.fda.gov/drugs/science-and-research-drugs/table-pharmacogenomic-biomarkers-drug-labeling
- Orrantia-Borunda E, Anchondo-Nuñez P, Acuña-Aguilar LE, Gómez-Valles FO, Ramírez-Valdespino CA. Subtypes of Breast Cancer. In: Mayrovitz HN, ed. Breast Cancer. Exon Publications; 2022.
- Masoud V, Pagès G. Targeted therapies in breast cancer: New challenges to fight against resistance. World J Clin Oncol. 2017;8(2):120-134. doi:10.5306/wjco.v8.i2.120
- Egbewande OM, Abdulwasiu MA, Yusuf RO, Durojaye AB, Ashimiyu-Abdulsalam ZI. Roles of community pharmacists in cancer management. Innov Pharm. 2022;13(3):10.24926/iip.v13i3.4946. doi:10.24926/iip.v13i3.4946
- Genetics of Prostate Cancer (PDQ). National Cancer Institute. Updated November 8, 2023. Accessed December 28, 2023. https://www.cancer.gov/types/prostate/hp/prostate-genetics-pdq
- LiverTox: Clinical and Research Information on Drug-Induced Liver Injury. National Institute of Diabetes and Digestive and Kidney Diseases; 2012.
- Barbieri CE, Bangma CH, Bjartell A, et al. The mutational landscape of prostate cancer. Eur Urol. 2013;64(4):567-76. doi:10.1016/j.eururo.2013.05.029
- McLean AEB, Barnes DJ, Troy LK. Diagnosing lung cancer: the complexities of obtaining a tissue diagnosis in the era of minimally invasive and personalised medicine. J Clin Med. 2018;7(7):163. doi:10.3390/jcm7070163
- Larsen JE, Minna JD. Molecular biology of lung cancer: clinical implications. Clin Chest Med. 2011;32(4):703-740. doi:10.1016/j.ccm.2011.08.003
- Yip HYK, Papa A. Signaling pathways in cancer: therapeutic targets, combinatorial treatments, and new developments. Cells. 2021;10(3):659. doi:10.3390/cells10030659
- Massarelli E, Papadimitrakopoulou V, Welsh J, Tang C, Tsao AS. Immunotherapy in lung cancer. Transl Lung Cancer Res. 2014;3(1):53-63. doi:10.3978/j.issn.2218-6751.2014.01.01
- Brothers KB, Rothstein MA. Ethical, legal and social implications of incorporating personalized medicine into healthcare. Per Med. 2015;12(1):43-51. doi:10.2217/pme.14.65
- Leighl NB, Nirmalakumar S, Ezeife DA, Gyawali B. An arm and a leg: the rising cost of cancer drugs and impact on access. Am Soc Clin Oncol Educ Book. 2021;41:1-12. doi:10.1200/EDBK_100028
- Debela DT, Muzazu SG, Heraro KD, et al. New approaches and procedures for cancer treatment: current perspectives. SAGE Open Med. 2021;9:20503121211034366. doi:10.1177/20503121211034366
- Pritchard DE, Moeckel F, Villa MS, Housman LT, McCarty CA, Mcleod HL. Strategies for integrating personalized medicine into healthcare practice. Per Med. 2017;14(2):141-152. doi:10.2217/pme-2016-0064
- Rulten SL, Grose RP, Gatz SA, Jones JL, Cameron AJM. The future of precision oncology. Int J Mol Sci. 2023;24(16):12613. doi:10.3390/ijms241612613
- Oprea TI, Bologa CG, Brunak S, et al. Unexplored therapeutic opportunities in the human genome. Nat Rev Drug Discov. 2018;17(5):317-332. doi:10.1038/nrd.2018.14
- Holle LM, Segal EM, Jeffers KD. The Expanding role of the oncology pharmacist. Pharmacy (Basel). 2020;8(3):130. doi:10.3390/pharmacy8030130
- Kennedy MJ. Personalized medicines - are pharmacists ready for the challenge? Integr Pharm Res Pract. 2018;7:113-123. doi:10.2147/IPRP.S133083